News
Article
Enhancing Patients' Motivation and Empowerment: A Resident’s Perspective
Empowerment has a significant correlation with patients’ overall mental and physical well-being, and has been central to the shift in conceptual framework of mental illness recovery towards a focus on resilience, strength, and control over one’s life.
Nuthawut/AdobeStock

Case Example
“Ms Smith” was admitted from the ER to the inpatient unit due to moderate major depressive disorder (MDD) and suicidal ideation. During intake the next day, she entered the interdisciplinary team meeting room with a low mood, flat affect, and lack of motivation. Despite encouragement, she could not provide any information about the events that led to her current hospitalization, acute stressors, and psychosocial history. Ms Smith was already experiencing defeatism, learned helplessness, and failure. Ms Smith’s presentation seemed standard in clinical settings. The treating psychiatrist and clinical team asked basic questions and ended the conversation with a typical “it is hard to manage emotions, but we are here to work with you.”How best we can deal with this case?
Empowering Patients
Due to underlying psychopathology, psychosocial stressors, and social determinants of health, individuals with mental illness are often vulnerable, skeptical, and may feel unempowered to improve their lives. The renowned monk and religious leader, Sadhguru, once eloquently asked a group of listeners, “When would you learn how to take care of your body, feelings, and emotions—in your 80s? When you will be no good for anything…” Additionally, Sadhguru highlights, “Our body is a user manual; have we ever attempted to read this user manual?” Building empowerment and enhancing motivation are not easy tasks due to time constraints during clinical visits, preference of clinicians, and resistance of patients to accept change. However, mental wellness can be improved by capacity building among vulnerable patient populations by establishing a robust therapeutic alliance; providing compassionate care; validating feelings; and motivating and encouraging patients to make conscious—not impulsive or compulsive—decisions. One of the essential elements of motivation is finding a purpose in life and uncovering what our patient values, which may include their family, employment, relationships, spirituality, or serving the community. Getting a deeper understanding of a patient's thoughts, emotions, and how it impacts their behaviors is crucial in clinical encounters.
Empowerment is quite literally defined as, “letting this power out.” It encourages individuals to gain the skills and knowledge to overcome obstacles in life or the workplace and to develop within themselves or in society. From the author’s perspective, our world needs robust leaders in the form of psychiatrists and therapists to lift those experiencing defeatism, anhedonia, and a lack of desire to live. Although any healer can play a pivotal role in empowering and motivating patients, the primary responsibility falls to mental health clinicians, as they encounter patients struggling with mental health challenges firsthand. Instead of simply accepting a patient’s lack of motivation or low drive, building a therapeutic alliance, transforming negativity with positivity, ambivalence with action, and installing hope for recovery should be the prime focus of the treatment team in an ideal world.
Encouraging patients to take their time and follow mindfulness techniques can produce highly desirable outcomes. Additionally, an essential component of empowerment includes teaching patients to use a systematic problem-solving strategy (eg, SOLVE, where S= Situation specified; O= Options listed with pros and cons; L= Listen to others; V= Voice a choice; I= implement an option; and E= evaluate the outcome).1
Close follow-up is mandatory to build consistent empowerment, resilience, and strength among the vulnerable population. Based on the patients’ interests and interactions, referrals can be made to motivational programs, if necessary. Additionally, questions about motivation and empowerment should be part of the daily assessment, and these factors should be measured using mental health-specific empowerment rating scales, such as the Empowerment Scale2 and the Mental Health Confidence Scale.3
Patients with mental health challenges often report negativity, ambivalence, and a lack of motivation. Several factors play roles in the psychopathology of their symptoms, such as significant reduction in neurotransmitters (dopamine, norepinephrine, serotonin), co-occurring substance use disorders, medical illnesses, and poor psychosocial support/deficits in social determinants of health. Implementing collaborative efforts among health care providers and empowering patients to take the lead on their health can reduce the burden of mental illnesses and will contribute to healthy communities.
Discussion
Empowerment has a significant correlation with patients’ overall mental and physical well-being,4 and has been central to the shift in conceptual framework of mental illness recovery towards a focus on resilience, strength, and control over one’s life.5,6 The strongest indicator for belonging to the group with the highest ratings on empowerment comes with a step-by-step collaborative approach to improving the mental status and psychological well-being of patients with mental illnesses.
Psychodynamic therapy emphasizes patients’ relationships and interpersonal experience (in theoretical terms, object relations, and attachment). To the extent that there are repetitive themes in a person’s relationships and manner of interacting, these themes tend to emerge in some form in the therapy relationship. For example, a person prone to distrust others may suspect the therapist. In contrast, a person who fears disapproval or abandonment may fear rejection by the therapist, whether knowingly or unknowingly. Another person who struggles with anger and hostility may struggle with anger toward the therapist.7 Moreover, building a self-efficacious and empowered relationship between therapist and patient is a crucial step that can become deeply meaningful and emotionally charged.
Providing an “empowering encounter” can help patients gain a new perspective on the cause and management of their emotional health issues via motivation and self-efficacy. Many patients need motivation and empowerment skills to develop a higher sense of insight and introspection, to mobilize hidden and inner abilities and energies, and to reflect upon their own cognitive and affective schemata. An empowering approach to psychotherapy may involve creating a focus on a patient’s strengths rather than weaknesses, assisting patients in constructing options for change, helping patients to identify thought patterns and understand consequences of behaviors, and supporting patients in developing a sense of control over their lives.The feeling of empowerment has been noted as essential to a positive psychotherapy experience, leaving patients with increased self-confidence and improved coping skills.8
Abraham Maslow’s Hierarchy of Needs
Figure. Abraham Maslow’s Hierarchy of Needs
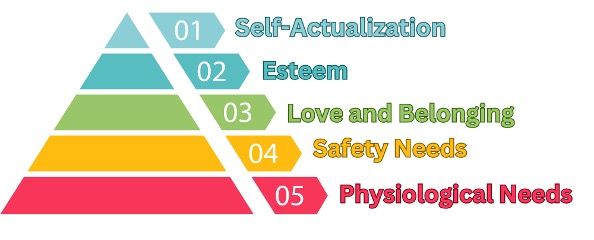
According to Abraham Maslow’s Hierarchy of Needs (Figure) and his theory of motivation, all human beings have a hierarchy entailing 5 essential needs, beginning with physiological well-being. Beyond physiological, there are safety, social, esteem, and self-actualization needs.
Maslow and Laski studied the psychology of creativity and drew parallels between creative situations and mystical experiences, linking the processes of self-discovery and self-actualization. Building comparable processes is vital in all clinical settings (ie, outpatient, inpatient, and crisis units). Clinicians should ask questions that will motivate and empower patients to live more productive lives (Table 1).
Table 1. Examples of Empowering Questions

Complicating the empowerment of patients is the self-evident truth that opportunities in life are not created equally, and patients with mental illness may not get the same opportunities as individuals without mental illness. For example, some patients with severe mental illness may have difficulty maintaining a career that achieves self-fulfillment. Each individual’s concept of self-actualization is integrally tied to their identity, which is molded by environment and significant life experiences. Thus, encouraging a patient to reach their own self-actualization inherently includes understanding the patient’s motivations and experiences, identifying their strengths and values, and empowering them to embrace their right to self-determination.9 When patients feel satisfied that their psychosocial needs are being addressed, they tend to feel a sense of self-confidence, prestige, empowerment, and control. As a result, individuals feel helpful, seek growth, and contribute to society.
Motivational Interviewing and Self-Determination Theory
Self-Determination Theory is useful for understanding how patient-centered communication and promotion of patient autonomy and empowerment can lead to positive health outcomes.10 As such, motivational interviewing plays a key role in creating a successful physician-patient relationship that encourages changes in maladaptive behaviors and thought patterns. Motivational interviewing techniques can empower patients to develop a sense of autonomy and create changes in behavior that aligned with their personal values.11 Motivational interviewing skills that promote physician-patient collaboration include integrating reflective statements, eliciting the patient’s values and factors that may drive them toward change, and determining the patient’s understanding or past use of resources to provide more relevant education.11
Interpersonal Communication in Psychodynamic Therapy
The psychoanalytical theory has been adapted to place more of an emphasis on interpersonal relationships and has provided a technique for understanding and interpreting human emotions, thoughts, behaviors, and past events reshaping personality.12 This approach provides a possibility in communication as it explains human beings’ contrary reactions toward similar situations. For example, when 2 individuals are conversing, their attitude toward a situation stems from a variance between conscious, preconscious, and unconscious minds. If a vulnerable person is being criticized, the slightest thought inside them may cause them to yell or scream at the individual criticizing them easily. However, for a more grounded individual, the preconscious part of their thought process influences their actions more prominently, and they may not act so impulsively or even be prone to listen attentively. The events that are stored in our unconscious minds mostly reshape our instinctive behavior. Examples of such events can be any trauma in childhood like sexual abuse or sudden death of a caregiver.
Maintaining effective open communication is key during clinical encounters. Additionally, understanding verbal and non-verbal cues is critical.Frequency of communication is usually driven by the frequency of therapy, level of therapeutic alliance, and patient willingness to share the information. Actively listening to patients’ perspectives gives patients a sense of being heard and improves patient mental health outcomes and self-efficacy.
The areas defining psychodynamic therapy, treatment hierarchy, role definition, theoretical clarity, and boundaries are often fluid, with considerable overlap. They are commonly in flux throughout a treatment course and require active communication as a glue to hold the treatment together and focus on a common goal.
Practicing Gratitude
One of the key factors in motivating patients is reminding them to practice gratitude. The benefits of practicing gratitude are endless. Individuals who regularly practice gratitude by noticing and reflecting upon the things they are thankful for experience less depressive symptoms,13 decreased stress,14 more positive emotions, improved sleep quality,15 and even physical health benefits.15 With gratitude, individuals acknowledge the goodness in their lives. Gratitude helps people relish good experiences, improve their health, deal with adversity, and build strong relationships. The 3 stages of gratitude can be seen in Table 2. The effects of gratitude can be important for overall well-being for several reasons, such as improved mental and physical health, stronger social bonds, and resilience.
Table 2. The 3 Stages of Gratitude

Shortage of Mental Health Providers
The significant shortage and inequitable distribution of psychiatrists and other mental health clinicians in the United States is one of the critical reasons for the large treatment gap for individuals with mental disorders. Patients may face challenges and obstacles in scheduling appointments, paying out of pocket, and lacking access to services. As appropriate, psychiatrists should support and assist colleagues who can administer effective interventions. As mental health leaders, psychiatrists should design and manage empowerment/motivation programs, build clinical capacity, provide supervision, ensure quality assurance, and follow up on different referral pathways and research. It is also fundamental that patients be involved in their educational programs so that the programs can be tailored and targeted to their needs and become more effective in their long-term recovery. Although challenging, collaborating with health care professionals to ensure continuity of care should be pursued.
Concluding Thoughts
Patients with mental health challenges may experience lack of motivation, low mood, and defeatism. Empowerment has a significant correlation with patients’ overall mental and physical well-being. It is crucial to motivate and empower patients during clinical encounters in addition to treatment with medications. Our world needs robust leaders in the form of psychiatrists and mental health providers to lift those experiencing defeatism, anhedonia, and lack of desire to live. The empowered leader can bring significant changes and improve patients’ well-being with the installation of hope and capacity-building among vulnerable patient populations. Future studies should focus on identifying how the process of motivating and empowering impacts patient clinical outcomes and benefits communities at large.
Dr Kumari is a psychiatry resident (PGY-4) at Hackensack Meridian Health Ocean University Medical Centre.
Ms Jenkins is a third year medical student at Hackensack Meridian School of Medicine in Nutley, New Jersey.
References
1. Berghuis DJ, Peterson LM, Burce TJ. The Complete Adult Psychotherapy Treatment Planner. Wiley; 2014.
2. Corrigan PW, Faber D, Rashid F, Leary M. The construct validity of empowerment among consumers of mental health services. Schizophr Res. 1999;38(1):77-84.
3. Carpinello SE, Knight EL, Markowitz FE, Pease EA. The development of the Mental Health Confidence Scale: a measure of self-efficacy in individuals diagnosed with mental disorders. Psychiatric Rehabilitation Journal. 2000;23(3):236.
4. Fitzsimons S, Fuller R. Empowerment and its implications for clinical practice in mental health: a review. Journal of Mental Health. 2002;11(5):481-499.
5. Khoury E, Rodriguez del Barrio L. Recovery-oriented mental health practice: a social work perspective. The British Journal of Social Work. 2015;45:i27-i44.
6. Leamy M, Bird V, Le Boutillier C, et al. Conceptual framework for personal recovery in mental health: systematic review and narrative synthesis. Br J Psychiatry. 2011;199:445-452.
7. Shedler J. The efficacy of psychodynamic psychotherapy. Am Psychol. 2010;65(2):98-109.
8. De Smet MM, Meganck R, De Geest R, et al. What “good outcome” means to patients: understanding recovery and improvement in psychotherapy for major depression from a mixed-methods perspective. J Couns Psychol. 2020;67(1):25-39.
9. Laser-Maira JA, Peach DM, Hounmenou CE. Moving towards self-actualization: a trauma-informed and needs-focused approach to the mental health needs of survivors of commercial child sexual exploitation. International Journal of Social Work. 2019;6(2).
10. Ng JY, Ntoumanis N, Thøgersen-Ntoumani C, et al. Self-determination theory applied to health contexts: a meta-analysis. Perspect Psychol Sci. 2012;7(4):325-340.
11. Sohl SJ, Birdee G, Elam R. Complementary tools to empower and sustain behavior change: motivational interviewing and mindfulness. Am J Lifestyle Med. 2016;10(6):429-436.
12. Kerr S, Goldfried M, Hayes A, et al. Interpersonal and intrapersonal focus in cognitive–behavioral and psychodynamic–interpersonal therapies: a preliminary analysis of the Sheffield Project. Psychother Res. 1992;2(4):266-276.
13. Harbaugh CN, Vasey MW. When do people benefit from gratitude practice? The Journal of Positive Psychology. 2014;9(6):535-546.
14. Tolcher K, Cauble M, Downs A. Evaluating the effects of gratitude interventions on college student well-being. J Am Coll Health. 2022;1-5.
15. Jackowska M, Brown J, Ronaldson A, Steptoe A. The impact of a brief gratitude intervention on subjective well-being, biology and sleep. J Health Psychol. 2016;21(10):2207-2217.
Newsletter
Receive trusted psychiatric news, expert analysis, and clinical insights — subscribe today to support your practice and your patients.






