Article
Challenging Patients
Author(s):
What factors lie at the heart of the patient/physician relationship?
Table 1
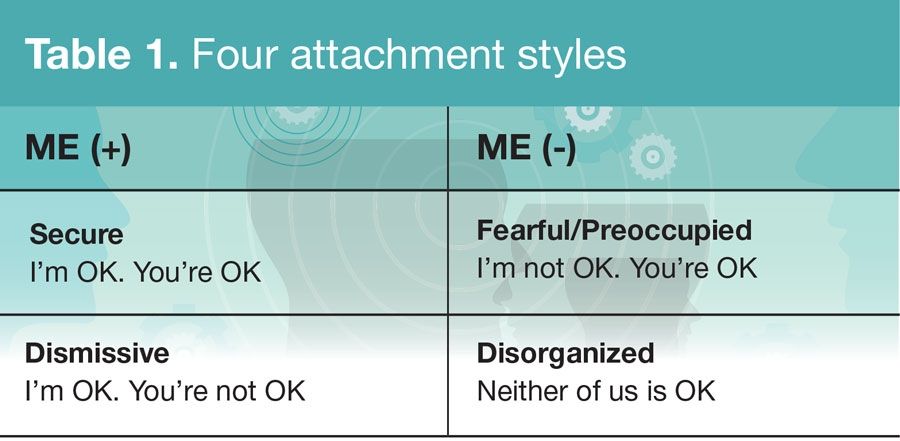
Table 2
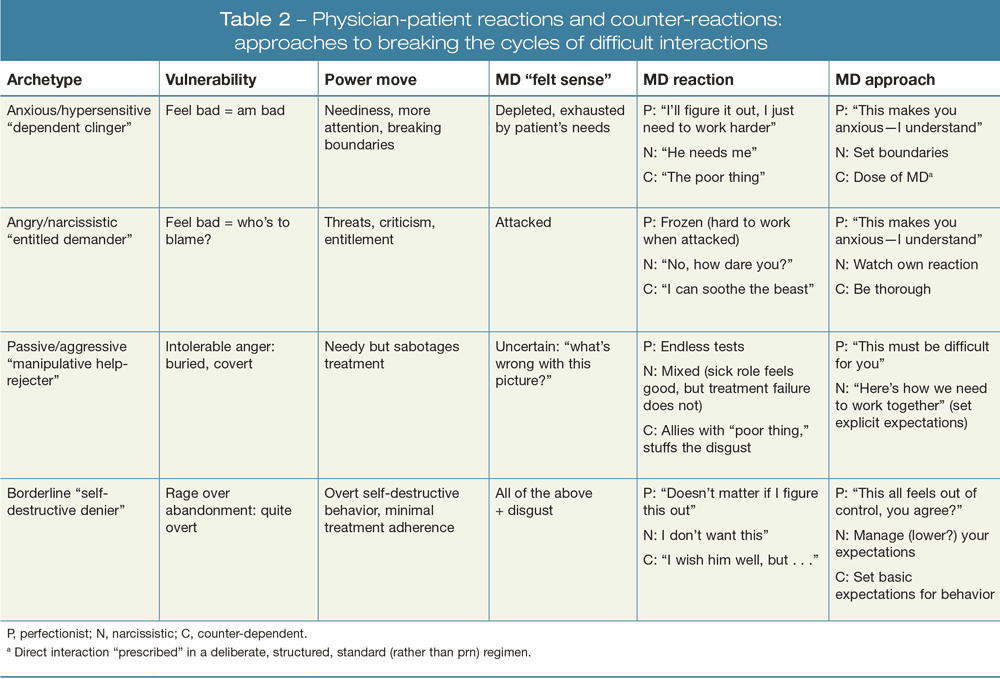
Good interpersonal communication is at the crux of the patient-physician relationship. Many factors come into play when the relationship breaks down. Understanding various personality types and how certain personalities and relationship archetypes influence physicians will be the focus of an interactive session at APA 2016.
Here are 3 questions that touch on some of the topics from that session.
QUESTION 1
Which of the following bests fits with a dismissive attachment style?
A. I’m OK, you’re OK
B. I’m OK, you’re not OK
C. I’m not OK, you’re OK
D. I’m not OK, you’re not OK
Answer 1: B.
"I’m OK, you’re not OK" bests fits with a dismissive attachment style.
Table 1 provides examples of four attachment styles.
Question 2
What is another way to describe the manipulative help-rejecting patient?
A. Borderline
B. Angry-narcissistic
C. Passive-aggressive
D. Anxious-hypersensitive
Answer 2: C.
Patients who are “manipulative help-rejecting”-ie, “passive-aggressive”-tend to be highly susceptible to others’ suggestions and catastrophize situations in their lives. They commonly challenge and violate the clinician’s time and space boundaries.
For example, they may routinely run over scheduled appointment times, initiate frequent “emergency” contact outside of office hours, and make limitless requests (eg, petition elaborate laboratory tests or the request the latest medication for routine ailments). (Table 2)
Table 2 from: Sazima G. The “Hateful Patient” Revisited: A Transactional View of Difficult Physician-Patient Relationships. Psychiatric Times. June 19, 2015.
Question 3
The “Chairperson’s syndrome” occurs with which of the following patients?
A. A physician admitted for an arthroscopic repair of the knee
B. A hospital vice-president admitted for ACS-3
C. A resident physician admitted with an acute myeloblastic crisis
D. An actress admitted for plastic surgery
Answer 3: D.
“Chairperson’s syndrome” is pressure for the VIP patient to be cared for by the department head. The pressure may come from the patient, family, or attendants, who may assume that the Chairperson is the best doctor for the clinical circumstance.
The pressure may also come from the Chairperson, who feels the need to “take command” in a situation with high visibility. Nevertheless, designation of a Chairperson to care for a VIP patient is appropriate only when the Chairperson is indeed the clinician who has the most expertise in the patient’s clinical issues.
For more information, see “The ‘Hateful Patient’ Revisited: A Transactional View of Difficult Physician-Patient Relationships,” by Greg Sazima, MD, on which Dr Muskin’s session and this article is based.
Further reading
• Groves JE. Taking care of the hateful patient. N Engl J Med. 1978;298:883-887.
• Smith MS, Shesser RF. The emergency care of the VIP patient. N Engl J Med. 1988;319:1421–1423.
Disclosures:
Dr Muskin is Professor of Psychiatry at Columbia University Medical Center, and Chief of Service: Consultation-Liaison Psychiatry, at New York-Presbyterian Hospital/Columbia University Medical Center in New York. He is an editorial board member of Psychiatric Times.
Newsletter
Receive trusted psychiatric news, expert analysis, and clinical insights — subscribe today to support your practice and your patients.






