Publication
Article
Psychiatric Times
Data-Driven: How Technology Can Improve Psychiatric Practice
Still in its infancy, the field of technology in psychiatry is rapidly growing and holding much promise in diagnosis, symptom tracking, behaviorial reinforcement, and a host of other useful tools.
metamorworks/AdobeStock

DIGITAL PSYCHIATRY
As smartphone ownership has skyrocketed and internet connectivity has become a necessity, patients and clinicians alike have seen the potential of evidence-based digital interventions. However, mainstream clinical practice has been slow to adopt these new technologies. Reluctance to use digital interventions might be related to attitude/familiarity, knowledge, and systemic/liability concerns.
The slow adoption may also be due to a lack of interdisciplinary dialogue between app users (the consumer, the patient, the physician), app makers/designers (engineers, computer scientists, and artificial intelligence experts), and the clinical practitioners. Currently, app and wearables data do not directly correspond to psychiatric diagnoses. Incorporating technology into mental health treatment plans could allow clinicians to work smarter, with continuously updated information. Clinicians and patients would benefit greatly from novel clinical workflows that incorporate apps and wearables as long as they meet confidentiality/privacy requirements. Innumerable patients have phones and other digital devices that could be gathering relevant information, but the information present in those devices has no formal role in clinical practice yet.
What Do Wearable Technologies Measure?
Wearables can include shirts, necklaces, headbands, wristbands, watches, shoes, and eyeglasses. They can be used to monitor physiological parameters such as temperature, heart rate, skin conductance, respiratory amplitude, and body movements, which may help monitor disease status.
Flexible biosensing is a rapidly growing industry and area of research. It aims to produce flexible material that can be worn as close to the skin as possible in a noninvasive and unobtrusive manner. These wearables can include physiological signal-monitoring sensors; customized designs with transmitters, receivers, filters, and circuit tracks—all with reduced size, lighter weight, and lower power consumption.1 Biosensing can also be used to measure chemical levels in the body, such as blood sugar, calcium, lithium, and oxygen saturation.2
In the field of psychiatry, only the more basic sensing aspects are eyed as adjuncts for information-gathering and digital therapeutics. Yet, even in their most basic form, sensors have the possibility of changing the way psychiatrists monitor their patients’ symptoms. Instead of relying on subjective information from patients, clinicians could gather objective data on sleep habits, activity levels, food intake, medication adherence, and even substance use. Onset of certain troubling patterns or departure from established baseline patterns serve as diagnostic cues. For instance, increases in motor activity (a proxy for agitation) can be a diagnostic prelude for mania.3
Key to success is the establishment of a clear relationship between the objective measure and the disease or mental health issue. For instance, irregular respiratory amplitude might signal decompensation of asthma. Since the link between shortness of breath and an asthma attack is well understood, a wearable looking at such data could theoretically be implemented.4 Turning to psychiatry, anxiety symptoms can occur in panic attacks and mimic asthma in an individual who has both disorders; in this case, irregular respiratory amplitude could signal worsening in either or both conditions. Interestingly, the wearable itself cannot make this determination and differentiate conditions unless an artificial intelligence algorithm gathers and interprets additional data points. A stepwise approach to this chain of events is portrayed in Figure 1.
A Closer Look at Smartphone-Provided Information
The data gathered by smartphones are comparable to wearables, because most individuals carry smartphones on them most of the time. Information provided by a phone or a wearable is referred to as passive sensing, requiring no action on behalf of the user. Below is a non-exhaustive summary of phone-measured dimensions. Note that wearable bands used for fitness cover much of the same information but may not share all of it with users.
The most basic data a phone can provide is GPS information. GPS location tracking provides a detailed image of a patient’s routine. Phones can also measure exposure to daylight, which can share information about the patients leaving their home. These 2 data points tell a story of isolation and psychomotor retardation, both potential indicators of worsening depression. Similarly, sleep fluctuations can be detected by examining screen on/off features and accelerometry data.
The use of text/SMS can establish an individual’s sociability baseline. How large is a patient’s social network? How many people do they interact with on a regular basis? How long do their conversations last, and do they prefer phone to text? Deviations from this baseline can be seen in mood disorders (ie, isolation and withdrawal in depression; extraversion and increased sociability in mania); psychotic disorders (ie, isolation and withdrawal with worsening paranoia or persecutory delusions); and anxiety disorders and substance use disorders (ie, calls at erratic times; increased activity; certain suspicious locations). The length and content of verbal and written communication can also be indicative of pathology or relapses.
Lastly, movement anomalies and tremors can also be detected with smartphone-based monitoring and can be useful in assessing medication adherence and effectiveness.5
Symptom Monitoring and Privacy and Confidentiality
The potential of technology to detect deviations in behavioral patterns is vast. However, privacy concerns are legitimate, and every effort needs to be made to protect individuals with mental illness, especially because they are a vulnerable population. For instance, could looking at interpersonal communications violate a patient’s privacy and confidentiality? Linguistic analysis and natural language processing indicate high correlations between in-person clinical ratings and blinded ratings based on social media data posts,6 as well as potential in discriminating unipolar from bipolar depression.7 On Reddit, sentiment analysis, personal pronouns, and semantic category analysis differentiated belonging to a mental health support group versus other nonmental health groups.8 Social media content has been looked at as a contender for collateral in mental health care.9 Accessing content of social media posts could be valuable in assessing and following mood disorders.
Looking at an individual’s conversations can be helpful in assessment and diagnosis of mood, psychotic disorders, and brain injuries, but carries risk of privacy invasion. Prosody assessment can help diagnose schizophrenia spectrum disorders by clarifying lexical and syntactic information.10 With privacy-preserving measures and no content analysis, our group has proven that depressive symptom severity correlates with decreased text/SMS and call durations and frequency.11,12 Privacy preserving analyses is more technically challenging, but may be more acceptable to patients in terms of sharing data and allowing speech recordings.
Ecological Momentary Assessment
Ecological momentary assessment (EMA) refers to data reported by an individual in close temporal proximity to an event, which can help avoid recall bias. The use of smartphones has allowed EMA collection of feelings, reactions, and other behavioral measures more frequently than before. Answers in response to a prompt asking about mood are useful, especially in correlation with objective data from wearables or phones. In contrast to passive sensing, EMA cannot be collected continuously.
In the field of mental health, EMA is often centered on reports of mood but can also include questions about suicidality, self-harm impulses, hallucinations, substance or alcohol use, physical activity, self-esteem, etc. Both random and scheduled sampling are options, and the more frequent data collections allow for finer granularity in understanding microprocesses that govern emotional and behavioral experiences. EMA can also play a role in shaping emotions or behaviors by increasing awareness and, thus, needs to be studied carefully for potential placebo-like effect.13
Choosing the right EMA is crucial to understanding the patient’s experience, just as choosing the right interview question can facilitate therapeutic alliance. In selecting apps,14 it is important to determine the goals. For example, would an event-contingent sampling (ie, asking a patient to log when they have cravings for a substance or urges to hurt themselves) be helpful? Is time-contingent sampling (ie, examining when things happen to rule out adverse effects or explore life occurrences on mood) a more appropriate option? EMA is also used to train artificial intelligence and deep learning algorithms to predict events, such as resurgence of auditory hallucinations or bad mood.15,16 Once the algorithm is trained, frequent EMA is no longer needed.
Putting Technology Into Action
Referred to as digital health, the ability to leverage technology for encouraging positive behaviors is an area that could revolutionize health care, especially in psychiatry.
Mental disorders are heterogenous. A divergence can exist between what a patient reports and what the psychiatrist sees (eg, mixed features in a manic episode). The following tips can help fit this phenomenology within EMA and passive sensing findings.
Carefully evaluate prospective apps.The app evaluation model available on the American Psychiatric Association’s website offers a helpful guide to clinicians wishing to evaluate such applications.17 Specifically, clinicians should consider:
- On which platforms/operating systems does the app work? Does it work on a desktop computer?
- Has the app been updated in the past 180 days?
- Is there a transparent privacy policy that is clear and accessible before use? Does the patient understand it?
- Does the app collect, use, and/or transmit sensitive data? How are the data stored, and is storage claimed to be secure?
- Is there evidence of specific benefit from academic institutions, end-user feedback, or research studies? (Note: Most apps do not, hence the difficulty in recommending specific ones.)
- Does the app have a clinical/recovery foundation relevant to your intended use?
- Does the app seem easy to use? How much battery and data does it consume?
- Can data be easily shared and interpreted in a way that is consistent with the stated purpose of the app?
Avoid making a diagnosis based on data points from an app.Psychiatric diagnosis is categorical and relies on specific symptoms for a predetermined duration as dictated by the DSM-5 or the International Classification of Diseases, Eleventh Edition. Wearables do not provide a diagnosis, but rather a set of data points. A symptom of depressed mood does not equate to major depression, nor does a hallucination equate to a formal thought disorder. In incorporating findings in your formulation, use the data as part of a full clinical picture. Discuss app findings with the patient while avoiding diagnostic labels.
Think dimensional, not categorical.Symptom remission is the goal of treatment, but symptoms occur along a continuous spectrum. Findings from an app can be invaluable in helping patients move from partial to full remission. For instance, although a patient with depression may present with an improved affect and grooming suggestive of remission, the curves from a mood app show persisting poor functioning and, therefore, incomplete improvement. In this case, the improvement may have reached a certain threshold, which is not enough for full functional recovery. The dimension of depressed mood is distinct from the construct of a depressive disorder.
Apps and wearables generate an overwhelming amount of data that require specialized processing with deep learning algorithms. Clinicians should start with dimensions in which they have been trained, such as psychomotor retardation to agitation, depressed mood, food intake, and sleep. However, it is clear that othertransdiagnostic dimensions can tell a lot about an individual’s functioning, even if they are not part of traditional psychiatric diagnostic criteria. Functional imaging studies have largely moved in this transdiagnostic, dimensional direction, and these include psychological concepts such as impulsivity, compulsivity, sociability, and other biomarkers chosen based on functional connectivity and biomarker data.
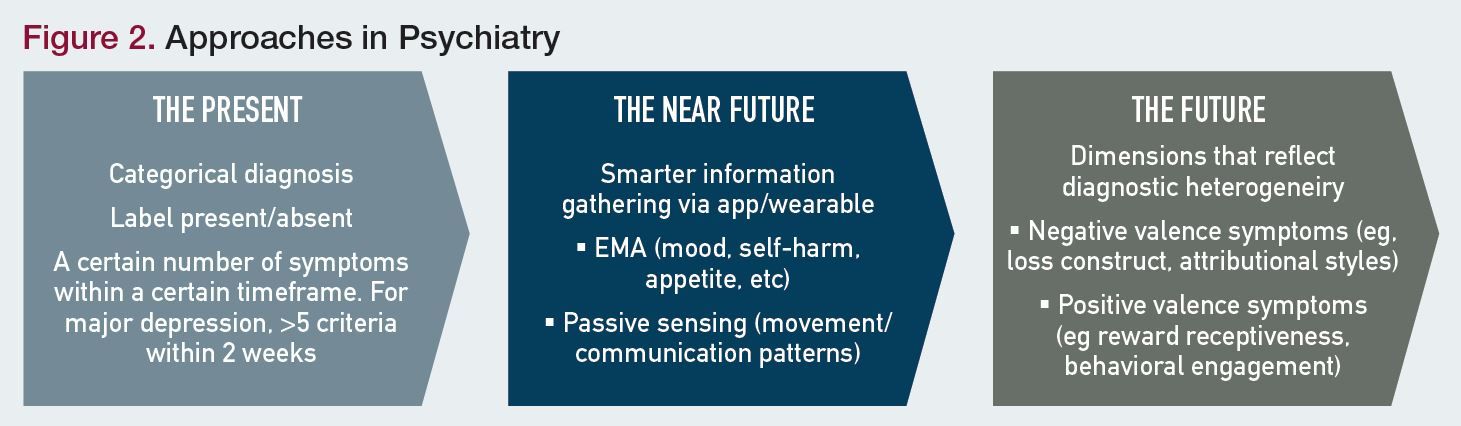
Figure 2 offers an example of dialogue between the categorical and dimensional approaches in psychiatry as mediated by wearable or app-provided information.
Use data from apps in session to discuss progress with your patients.Data collected outside of appointments offer a glimpse into the patient’s real life. In initiating use of any app or wearable, discuss the expectations and lay the foundation with the patient in terms of what the technology can do and cannot do. Then, during a later appointment, ask the patient to show you their mood graphs, and use this information to initiate a dialogue on noted bad days, triggers, sleep pattern deviation, etc.
There is rapid turnover of apps and technology, with few applications withstanding the test of time. As such, it is difficult to recommend any particular application, but it is useful to know the main ones in the field. Examples include Daylio and T2 Mood Tracker for journaling; Woebot, CBT coach, and CBT-I Coach for cognitive behavioral basics and insomnia; and Calm and Youper for wellness. A clinician familiar with an app can better guide the conversation.
Concluding Thoughts
Technology can be useful as adjunct to information gathering, diagnostic clarification, symptom tracking, and teaching/reinforcing behaviors for patients with mental illness. Still in its infancy, this exciting field is rapidly growing and holding much promise.
Case Vignette
“Julie” is a young adult with depression. Pharmacological management has helped somewhat, but the patient reveals urges to self-harm and continued intermittent depressive symptoms. However, Julie is not fully open about this issue. Financial considerations and transportation issues preclude the addition of psychotherapy and more frequent visits. Interestingly, Julie wears a fitness band. At one of the appointments, you suggest looking at her sleep results and note a particular Thursday and Friday have a more interrupted pattern than other days. Upon closer inquiry, Julie reports alcohol binging on those days.
With this in mind, you suggest she install a cognitive behavioral therapy app for substance use (reSET, which is FDA-approved), and plan for closer follow-up visits.
Dr Moukaddam is associate professor, Menninger Department of Psychiatry & Behavioral Sciences, Baylor College of Medicine and Ben Taub Adult Outpatient Services Director, Medical Director, Stabilization, Treatment & Rehabilitation (STAR) Program for Psychosis. Dr Sabharwal is chair of the Department of Electrical and Computer Engineering and the Earnest Dell Butcher professor of engineering at Rice University.
References
1. Sreenilayam SP, Ahad IU, Nicolosi V, et al. Advanced materials of printed wearables for physiological parameter monitoring. Materials Today. 2020;32:147-177.
2. Mukhopadhayay SC, Islam T. Wearable sensors for physiological parameters measurement: physics, characteristics, design and applications. In: Mukhopadhayay SC, Islam T, eds. Wearable Sensors. IOP Publishing; 2017.
3. Faurholt-Jepsen M, Vinberg M, Frost M, et al. Smartphone data as an electronic biomarker of illness activity in bipolar disorder. Bipolar Disord. 2015;17(7):715-728.
4. Alam R, Peden D, Lach J. Wearable respiration monitoring: interpretable inference with context and sensor biomarkers. IEEE J Biomed Health Inform. Published online July 6, 2020.
5. Kuosmanen E, Wolling F, Vega J, et al. Smartphone-based monitoring of Parkinson disease: quasi-experimental study to quantify hand tremor severity and medication effectiveness. JMIR Mhealth Uhealth. 2020;8(11) :e21543.
6. Kelly DL, Spaderna M, Hodzic V, et al. Blinded clinical ratings of social media data are correlated with in-person clinical ratings in participants diagnosed with either depression, schizophrenia, or healthy controls. Psychiatry Res. 2020;294:113496.
7. Mariani R, Di Trani M, Negri A, Tambelli R. Linguistic analysis of autobiographical narratives in unipolar and bipolar mood disorders in light of multiple code theory. J Affect Disord. 2020;273:24-31.
8. Low DM, Rumker L, Talkar T, et al. Natural Language Processing Reveals Vulnerable Mental Health Support Groups and Heightened Health Anxiety on Reddit During COVID-19: Observational Study. J Med Internet Res. 2020;22(10):e22635.
9. Yoo DW, Birnbaum ML, Van Meter AR, et al. Designing a clinician-facing tool for using insights from patients’ social media activity: iterative co-design approach. J Med Internet Res. 2020;22(10).
10. Lucarini V, Grice M, Cangemi F, et al. Speech prosody as a bridge between psychopathology and linguistics: the case of the schizophrenia spectrum. Front Psychiatry. 2020;11:531863.
11. Cao J, Truong AL, Banu S, et al. Tracking and predicting depressive symptoms of adolescents using smartphone-based self-reports, parental evaluations, and passive phone sensor data: development and usability study. JMIR Ment Health. 2020;7(1).
12. Moukaddam N, Truong A, Cao J, et al. Findings from a trial of the Smartphone and Online Usage-based eValuation for Depression (SOLVD) application: what do apps really tell us about patients with depression? Concordance between app-generated data and standard psychiatric questionnaires for depression and anxiety. J Psychiatr Pract. 2019;25(5):365-373.
13. Shiffman S, Stone AA, Hufford MR. Ecological momentary assessment. Annu Rev Clin Psychol. 2008;4(1):1-32.
14. Doherty K, Balaskas A, Doherty G. The design of ecological momentary assessment technologies. Interact Computers. 2020;32(3):257-278.
15. Li B, Sano A. Early versus late modality fusion of deep wearable sensor features for personalized prediction of tomorrow’s mood, health, and stress. Annu Int Conf IEEE Eng Med Biol Soc. 2020;2020:5896-5899.
16. Tseng VW, Sano A, Ben-Zeev D, et al. Using behavioral rhythms and multi-task learning to predict fine-grained symptoms of schizophrenia. Sci Rep. 2020;10(1):15100.
17. App Advisor. American Psychiatric Association. Accessed January 18, 2021. https://www.psychiatry.org/psychiatrists/practice/mental-health-apps ❒

Newsletter
Receive trusted psychiatric news, expert analysis, and clinical insights — subscribe today to support your practice and your patients.