Publication
Article
Psychiatric Times
Implementation Challenges of Universal Suicide Risk Screening in Adult Patients in General Medical and Surgical Settings
Author(s):
The authors share evidence-based guidance for patient safety that minimizes suicide risk in medical settings.
©Mindmo/Shutterstock

FROM THE ACADEMY OF CONSULTATION-LIAISON PSYCHIATRY
Suicide is a global public health crisis and is the 10th leading cause of death in the US.1 In 2018, more than 45,000 adults in the US died by suicide, surpassing the number of homicides by more than 2-fold. Moreover, suicide risk is even higher among individuals with comorbid medical illnesses. Illness such as cancer, diabetes, and asthma have all been shown to increase risk for suicide.2 Given that medical illness is a concerning suicide risk factor, medical settings provide an optimal venue for suicide risk detection and intervention.
Medical settings are well positioned to detect suicide risk. The majority of people who died by suicide visited a health care professional months before their death, placing medical providers on the frontlines of suicide risk detection and suicide prevention.3 However, many patients with suicidal thoughts who present to the health care system with somatic complaints do not disclose suicidal thinking unless asked directly, and most medical settings do not screen for suicide risk.4,5
Notably, suicides in the hospital are one of the top 5 most frequently reported sentinel events to The Joint Commission (TJC).6 Many are surprised to learn that although in-hospital suicides are relatively rare for patients undergoing general medical care, a sizeable portion of them occur on non-behavioral health units, such as intensive care units or emergency departments (EDs). Given these striking statistics and the goal of leveraging hospitals as partners in suicide prevention, TJC revised National Patient Safety Goal 15.01.01 (NPSG 15) in 2019.7 NPSG 15 outlines several elements to optimize patient safety and the reduction of suicide risk in medical settings. In particular, NPSG requires performing environmental safety assessments, removing ligature risks, screening patients with behavioral health issues for suicide risk, and providing further assessment of at-risk individuals who screen positive.7 Although NPSG 15 refers to suicide risk screening of all patients who are being treated or evaluated for a behavioral health condition as their primary reason for care, the TJC issued Sentinel Event Alert 56 in 2016, recommending suicide risk screening for all patients, using brief, evidence-based screening tools.8
Universal suicide risk screening
Following these recommendations, a growing number of health care systems have implemented suicide risk screening programs for all patients, including those presenting with medical complaints. Such a program at Parkland Health and Hospital System (PHHS) is an example of how to successfully implement hospital-wide universal suicide risk screening. Using one of the screening tools recommended by TJC, PHHS screened more than 325,000 patients in the first 6 months of implementing their screening program and detected a positive screen rate of below 4% among patients undergoing medical care.9 It will be important for hospitals to work with frontline clinicians to develop safe and feasible procedures for implementing the safety guidelines outlined in NPSG 15 across diverse rural and urban settings and to be able to articulate their procedures to TJC surveyors when they assess hospitals for safe care delivery.
Suicide risk screening tools
Several suicide risk screening tools are commonly used, with varying levels of evidence to support their use among these patients. Thom and colleagues10 reviewed several brief suicide risk screening tools and discussed the benefits and limitations of each for use in a hospital setting.10 Their review discusses 6 screening tools, including the Ask Suicide-Screening Questions (ASQ), the Patient Safety Screener (PSS-3), and the Columbia-Suicide Severity Rating Scale (C-SSRS), most of which are also TJC-recommended screening tools.11-14 The authors highlighted that only 2 of the tools discussed, the ASQ and the PSS-3, were developed and validated specifically for patients undergoing medical care.
Notably, the C-SSRS, a tool used by many hospitals due to its application to both youth and adults, has not been validated specifically for use in medical settings. Although Thom and colleagues highlighted that no suicide risk screening tools have been validated for use among both pediatric and adult patients undergoing medical care, recent data show that the ASQ, originally validated for use among youth, also has excellent psychometric properties among adult medical patients, potentially allowing for the use of 1 screening tool across hospitals.15
Some medical settings utilize depression screeners to identify patients at risk for suicide. For example, the Patient Health Questionnaire (PHQ-9), which is an excellent depression screen, is sometimes utilized as a suicide-risk screening tool.10,14,16 Although there is a well-documented association between suicide and depression, extant research shows that the 2 are not synonymous. In 1 study, 90% of suicide decedents met criteria for diagnosis of a mental illness; however, only 28% of suicide decedents met the criteria for major depressive disorder.17 Moreover, screening solely for depression in patients undergoing medical care may not adequately detect suicidal ideation.18
Question 9 on the PHQ-9, which asks about the frequency of a patient being bothered by “thoughts that you would be better off dead, or of hurting yourself in some way,” contains both an “or” and the word hurting instead of killing. Some studies have used this item to identify large numbers of at-risk patients.19,20 However, specific concerns exist regarding the sensitivity and specificity of item 921,22; the awkward wording of the question leading to inaccurate responses23; and that relying solely on item 9 may miss a large portion of patients at risk for suicide.24,25
Using depression screeners such as the PHQ-9 as a proxy for suicide risk screening may be insufficient to detect suicide risk. Additionally, other mental health disorders, such as substance use disorders, schizophrenia, and anxiety disorders are associated with risk of suicide, which would go undetected by screening only for depression.17 Asking directly about suicide risk and using validated tools specific to hospital settings is necessary to accurately screen for suicide risk.
In addition to being 1 of 2 suicide risk screening tools that was created and tested specifically for use among patients undergoing medical care, the ASQ is also part of a 3-tiered suicide risk screening clinical pathway.26 Although this pathway was designed for use among youth, the 3-tiered system can be applied to all such patients, including adults. The proposed pathway starts with the use of a brief screening instrument to rapidly screen all medical patients for suicide risk. For this step, Brahmbhatt and colleagues26 recommended the use of the ASQ due to its brevity and focus on patients undergoing medical care. The PSS-3 is the other screening tool that has been tested on adult patients in the ED and makes an excellent first-line brief screener.
Risk assessment
After a patient screens positive for suicide risk, the second and essential step is to have a trained clinician (eg, a mental health clinician, nurse practitioner, physician assistant, primary care physicians) conduct a 10- to 15-minute brief suicide safety assessment (BSSA) to determine how to effectively manage the patient’s suicide risk. The secondary safety assessment step was created to avoid a one-size-fits-all planfor anyone who screens positive on a primary screener. All positive screens should not be treated as an emergency; in fact, the majority of positive screens will be non-acute positives that do not require full safety precautions, but rather need further assessment.
This second step helps to ensure that mental health resources are used effectively and patients who reveal suicidal thoughts are not treated in a way that may seem punishing. For the BSSA, the clinical pathway published by Brahmbhatt and colleagues suggested the C-SSRS or the ASQ BSSA. Anecdotal evidence from frontline screeners suggests that the C-SSRS, which is a good in-depth suicide risk severity rating scale, is lengthy as a first-line screener and is more appropriate as a secondary suicide safety assessment tool for use among patients who screen positive for suicide risk. The ASQ and the ASQ BSSA are available as part of the ASQ Toolkit.27 The aim of the BSSA is to help a clinician further assess suicide risk in order to determine next steps in the pathway—whether a full mental health evaluation is needed at that particular medical visit, or if it can wait for an outpatient mental health referral.
Safety planning and counseling
Following a positive suicide risk screen, an essential component of ensuring patient safety is safety planning and lethal means counseling. Stanley and Brown28 published a safety plan worksheet that can help clinicians assist patients in planning how they will handle a future suicidal crisis. This worksheet consists of 6 steps that includes identifying personal warning signs, internal coping strategies, people and settings that can provide distraction, trusted people who can provide help, contact information for mental health resources, and ways to make the environment safe. The last step refers to the process of lethal means safety counseling, which is a detailed discussion on how to limit access, remove, or safely store dangerous items (eg, pills, firearms, knives, and ropes).
Implementation of suicide risk screening has been a specific challenge for many hospital systems due to difficulty selecting an evidence-based tool across the lifespan and across medical/surgical specialty settings that work in both inpatient and outpatient settings. In addition, guidance around how positive screens should be interpreted have led to systems developing untenable rules, such as “all positive screens require 1-to-1 sitters” and “strict safety precautions.”
Somewhat surprisingly, the rate of positives screen results due to reporting a past suicide attempts is significant. Past suicidal behavior is one of the most predictive risk factors of future behavior, but many reported attempts were in the distant past (eg, more than 10 years earlier). How should these truthful responses be interpreted? Such past behavior may be important clinical history when delivering a poor medical prognosis to a patient. Clearly more implementation research is needed on how to handle past attempt history and how frequently patients should be screened.
The impact of COVID-19
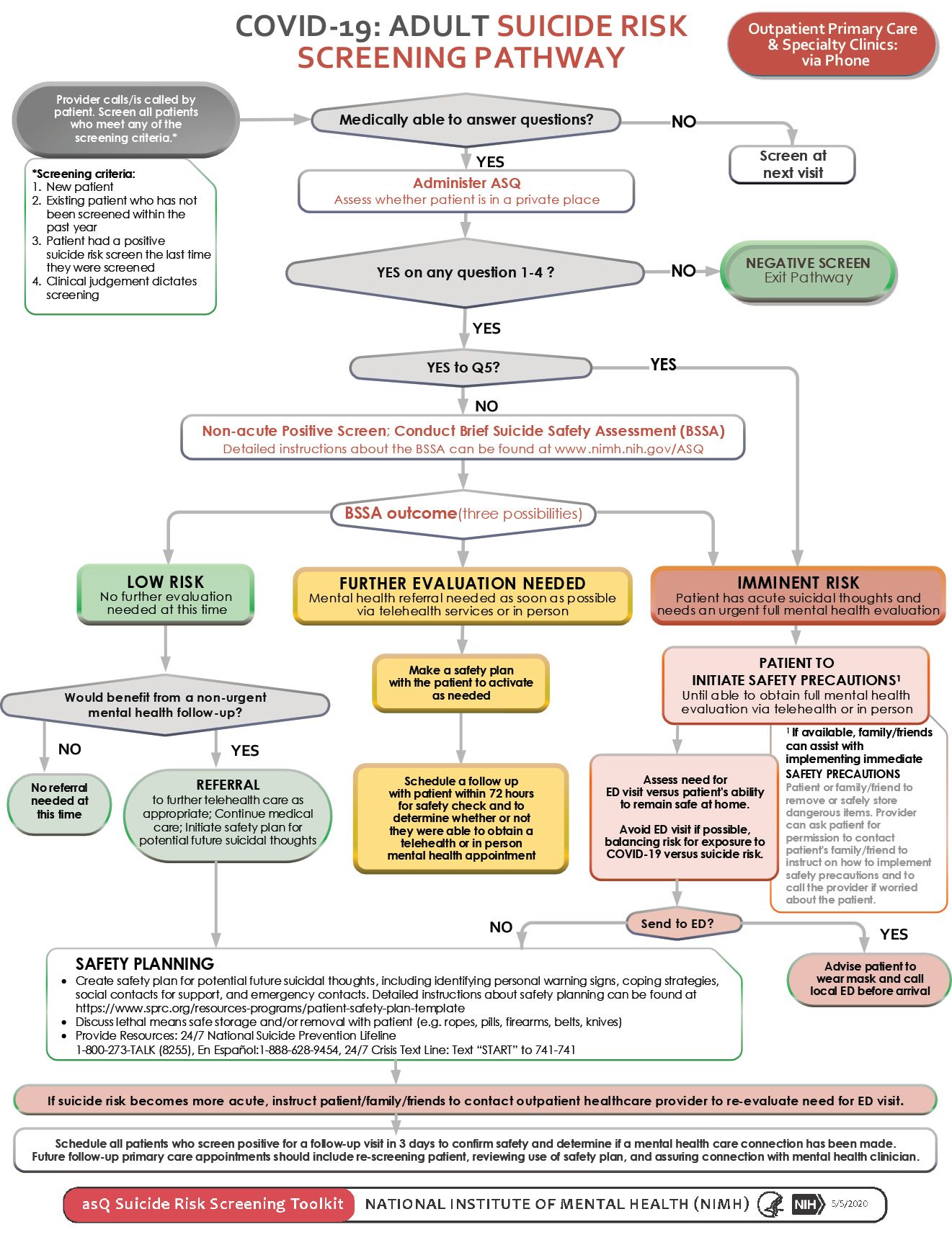
Suicide risk screening is especially challenging in the time of a pandemic. Data are not yet available to ascertain how COVID-19 will affect the suicide rate. However, the 3-tiered clinical pathway needed to be revised to accommodate mostly telehealth screening. Due to the urgent need, we revised the suicide risk screening clinical pathways published by Brahmbhatt and colleagues to reflect the need for phone screening and assessments.
Typically, anyone who is in imminent danger requires an urgent psychiatric evaluation in an ED. The pathway needed to be revised to help patients with acute suicide risk avoid exposure to COVID-19 in the ED and to spare the ED from over-crowding during the pandemic crisis. Separate adult and youth versions of this pathway were created and are available as part of the ASQ Toolkit (Figure).27 However, they have not yet been empirically tested. A critical part of this pathway is for the health care practitioner to provide lethal means counseling to the patient and family members or friends to ensure safe storage or removal of potentially dangerous items (eg, pills, firearms, belts, knives).
Conclusion
Detection and management of suicide risk screening in the medical setting is no longer theoretical. There are many hospitals successfully implementing suicide-risk screening programs with validated instruments. Universal suicide risk screening can be successfully implemented without incurring a need for additional resources. Use of the intermediate step of a brief suicide safety assessment provides critical guidance for determining appropriate follow up in a safe and efficient manner. Given the increasing suicide rates in the general population, medical venues offer important opportunities for early detection, assessment, and referral. With evidence-based tools and pathways to guide them, every health care provider can be a partner in suicide prevention.
Dr Pao is the Clinical Director of the National Institute of Mental Health (NIMH) Intramural Research Program at the National Institutes of Health, she is also the Deputy Scientific Director, NIMH; Ms Mournet is an Intramural Research Training Award Fellow at the NIMH; Dr Horowitz is a Staff Scientist and Clinical Psychologist at the National Institute of Mental Health Intramural Research Program at the National Institutes of Health, she also serves as a senior attending with a specialty in pediatric psychology on the Psychiatry Consultation Liaison Service in the Hatfield Clinical Research Center at NIH.
Acknowledgement—This research was supported in part by the Intramural Research Program of the NIMH (Annual Report Number ZIAMH002922).
References
1. CDC National Center for Injury Prevention and Control: Web-based Injury Statistics Query and Reporting System (WISQARS). cdc.gov/injury/wisqars/index.html. Accessed April 1, 2020.
2. Karmakar C, Luo W, Tran T, et al. Predicting risk of suicide attempt using history of physical illnesses from electronic medical records. JMIR Ment Health. 2016;3:e19.
3. Ahmedani BK, Stewart C, Simon GE, et al. Racial/ethnic differences in health care visits made before suicide attempt across the United States. Med Care. 2015;53:430–435.
4. Pan YJ, Lee MB, Chiang HC, Liao, SC. The recognition of diagnosable psychiatric disorders in suicide cases’ last medical contacts. Gen Hosp Psychiatry. 2009;31:181-1843.
5. Frankenfield DL, Keyl PM, Gielen A, et al. Adolescent patients”: healthy or hurting? Missed opportunities to screen for suicide risk in the primary care setting. Arch Pediatr Adolesc Med. 200;154:162-168.
6. The Joint Commission. Summary Data of Sentinel Events Reviewed by The Joint Commission. https://www.jointcommission.org/assets/1/18/Summary_4Q_2017.pdf. Accessed April 1, 2020.
7. The Joint Commission. Hospital National Patient Safety Goals. NPSG.15.01.01. https://www.jointcommission.org/-/media/tjc/documents/standards/national-patient-safety-goals/npsg_chapter_hap_jan2020.pdf. Accessed April 1, 2020.
8. The Joint Commission. Detecting and treating suicide ideation in all settings. Sentinel Event Alert. 2016;56:1-7.
9. Roaten K, Johnson C, Genzel R, et al. Development and implementation of a universal suicide risk screening program in a safety-net hospital system. Jt Comm J Qual Patient Saf. 2018;44:4-11.
10. Thom R, Hogan C, Hazen E. Suicide-risk screening in the hospital setting: A review of brief validated tools. Psychosomatics. 2020;61;1-7.
11. Horowitz LM, Bridge JA, Teach SJ, et al. Ask Suicide-Screening Questions (ASQ): a brief instrument for the pediatric emergency department. Arch Pediatr Adolesc Med. 2012;166):1170-1176.
12. Boudreaux ED, Jaques ML, Brady KM, et al. The patient safety screener: validation of a brief suicide-risk screener for emergency department settings. Arch Suicide Res. 2015;19:151-160.
13. Posner K, Brown GK, Stanley B, et al. The Columbia-Suicide Severity Rating Scale: initial validity and internal consistency findings from three multisite studies with adolescents and adults. Am J Psychiatry. 2011;168:1266-1277.
14. The Joint Commission. Validated/ Evidence-Based Screening Tools. Suicide Prevention Resources to support Joint Commission Accredited organizations implementation of NPSG 15.01.01. https://www.jointcommission.org/-/media/tjc/documents/resources/patient-safety-topics/suicide-prevention/suicide_prevention_resources_ep2_npsg150101.pdf. Accessed April 1, 2020.
15. Horowitz LM, Snyder DJ, Boudreaux ED, et al. Validation of the Ask Suicide-Screening Questions (ASQ) for adult medical inpatients: a brief tool for all ages. Psychosomatics. 2020;S0033-3182(20)30120-1.
16. Kroenke K, Spitzer RL, Williams JB. The PHQ-9: validity of a brief depression severity measure. J Gen Intern Med. 2001;16:606-613.
17. Conwell Y, Duberstein PR, Cox C, et al. Relationships of age and axis I diagnosis in victims of completed suicide: a psychological autopsy study. Am J Psychiatry. 1996;153:1001-1008.
18. Recklitis CJ, Lockwood RA, Rothwell MA, Diller LR. Suicidal ideation and attempts in adult survivors of childhood cancer. J Clin Onc. 2006;24:3852-3857.
19. Simon GE, Coleman KJ, Rossom RC, et al. Risk of suicide attempt and suicide death following completion of the Patient Health Questionnaire depression module in community practice. J Clin Psychiatry. 2016;77:221-227.
20. Simon GE, Rutter CM, Peterson D, et al. Does response on the PHQ-9 depression questionnaire predict subsequent suicide attempt or suicide death? Psychiatr Serv. 2013;64:1195-1202.
21. Uebelacker LA, German NM, Gaudiano BA, Miller IW. Patient health questionnaire depression scale as a suicide screening instrument in depressed primary care patients: a cross-sectional study. Prim Care Companion CNS Disord. 2011;13:PCC.10m01027.
22. Suarez L, Beach SR, Moore SV, et al. Use of the Patient Health Questionnaire-9 and a detailed suicide evaluation in determining imminent suicidality in distressed patients with cardiac disease. Psychosomatics. 2015;56:181-189.
23. Razykov I, Hudson M, Baron M, Thombs BD. Utility of the Patient Health Questionnaire?9 to assess suicide risk in patients with systemic sclerosis. Arthritis Care Res. 2013;65:753-758.
24. Louzon SA, Bossarte R, McCarthy JF, Katz IR. Does suicidal ideation as measured by the PHQ-9 predict suicide among VA patients? Psychiatr Serv. 2016;67:517-522. doi:
25. Dueweke AR, Marin MS, Sparkman DJ, Bridges AJ. Inadequacy of the PHQ-2 depression screener for identifying suicidal primary care patients. Fam Syst Health. 2018;36:281.
26. Brahmbhatt K, Kurtz BP, Afzal KI, et al. Suicide-risk screening in pediatric hospitals: Clinical pathways to address a global health crisis. Psychosomatics. 2019;60:1-9.
27. National Institute of Mental Health. Ask Suicide-Screening Questions (ASQ) Toolkit, 2017. https://www.nimh.nih.gov/ASQ. Accessed April 1, 2020.
28. Stanley B, Brown GK. Safety Planning Intervention: a brief intervention to mitigate suicide risk. Cogn Behav Pract. 2012;19:256-264.❒

Newsletter
Receive trusted psychiatric news, expert analysis, and clinical insights — subscribe today to support your practice and your patients.