Check out the pipeline updates from April!


Check out the pipeline updates from April!

A groundbreaking study explores innovative neuroassessment technology to enhance understanding and treatment of borderline personality disorder symptoms.

Here are 4 means of coping with the diagnostic uncertainty of bipolar mixed states.

Is the complex posttraumatic stress disorder diagnosis being used to avoid the diagnosis of borderline personality disorder?

Whether a patient has a diagnosis of cPTSD, BPD, or some combination of both, treatment should be considered multifaceted and overlapping. Learn more in this Special Report article.

Here are highlights from the week in Psychiatric Times.

Here's a look at the characteristic methods of communication among patients with BPD.

The experts weighed in on a wide variety of psychiatric issues for the April issue of Psychiatric Times.

Here are highlights from the week in Psychiatric Times.
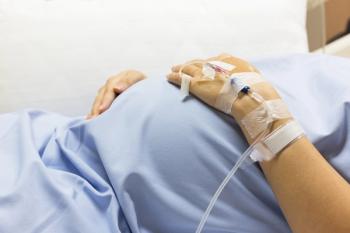
How can consultation-liaison psychiatry help identify BPD and facilitate effective communication between patients and medical teams during these patients’ admissions?

From personality disorders and common comorbidities to the effects of abortion bans on mental health, here are highlights from the week in Psychiatric Times.

In this CME article, examine the etiology of poor medical outcomes in borderline personality disorder and learn more about the assessment and management of patients with reported borderline personality disorder who have been admitted medically.

Given the paradoxical nature of borderline personality disorder, double bind communication appears to be a common method of engagement which ultimately serves only self-defeating purposes.

From a look at adolescent substance use to special challenges in treating borderline personality disorder during the perinatal period, here are highlights from the week in Psychiatric Times.

How can BPD traits affect the transition to parenthood?

PME affects many women, yet it remains under-recognized in clinical practice and in research.

What do the United States and borderline personality disorder have in common?

Mothers with borderline personality disorder often have experienced early-life trauma. How can you help?

Borderline personality disorder is a common diagnosis among young women that is highly understudied in pregnancy and motherhood. Learn more here.

Sleep disturbances in borderline personality disorder are relatively unrecognized.

These 3 essential steps best support patients with borderline personality disorder, according to Carl Fleisher, MD.

A patient presents with multiple substance use disorders super-imposed on mood and anxiety disorders. Where does a clinician even begin?

What do functional magnetic resonance neuroimaging findings reveal about the neurobiology of borderline personality disorder? Take the quiz and learn more.

Do personality disorders get a bad rap? Take the quiz and learn more.
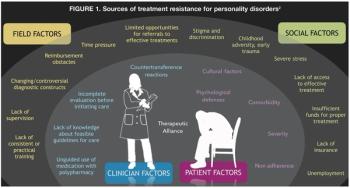
While treatment of bipolar disorder challenging , the notion that it is treatment resistant is contradicted by longitudinal and treatment research that indicates high rates of remission over time, moderate rates of recovery, and significant response to structured treatments tailored to symptoms.