Article
Differentiating Comorbid Bipolar Disorder and OCD
Author(s):
This review highlights an important diagnostic and therapeutic task: the importance of differentiating true bipolar disorder/obsessive-compulsive disorder comorbidity from BD with secondary OCD.

SPECIAL REPORT: OCD AND RELATED DISORDERS
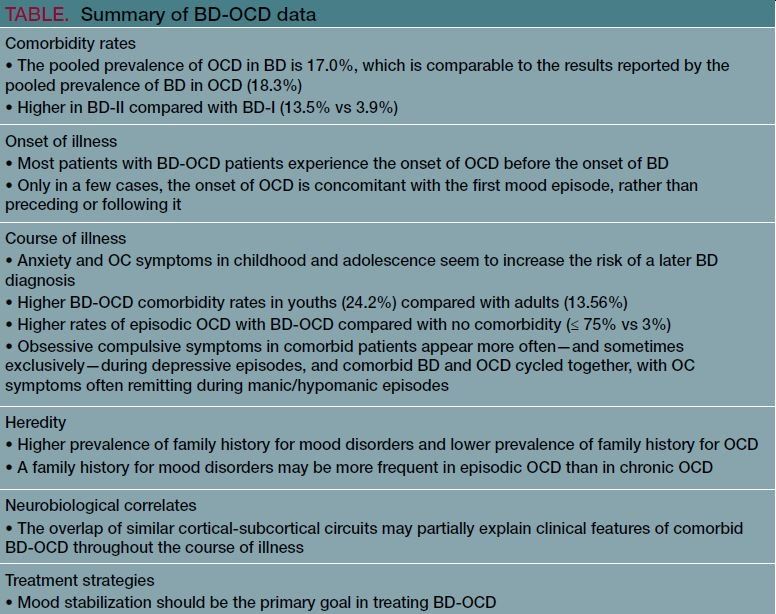
• BD-OCD comorbidity’s burden and clinical management is a critical issue in psychiatry.
• The evidence so far on BD-OCD nosology, which is mainly based on the course of illness, supports the view that the majority of cases of comorbid BD-OCD are in fact BD cases. Obsessive-compulsive symptoms usually are secondary manifestations of depressive or manic mood episodes.
• Mood stabilization should be the primary goal in treating patients with BD-OCD. Because of the risk of worsening BD via serotonin reuptake inhibitors-induced mania/hypomania, antidepressants should only be used in a minority of cases of refractory OCD.
In a classic 1970 publication, the famous epidemiologist Alvan R. Feinstein, MD, defined comorbidity in relation to a specific index condition as “any distinct additional entity that has existed or may occur during the clinical course of a patient who has the index disease under study.”1 In Feinstein’s formulation, the implication was that a completely different and independent disease occurred at the same time as another disease. These two diseases co-occurred, more often than not, randomly.
On the other hand, DSM explicitly offers overlapping clinical criteria for many diagnoses, especially mood and anxiety disorders, guaranteeing comorbidity in quite a different sense than in the medical meaning of the term as co-occurrence of independent diseases. Using the DSM definition, it is unclear whether concomitant diagnoses actually reflect the presence of distinct clinical entities or refer to multiple manifestations of a single clinical entity.
A little bit of history
A good example of this problem is the comorbidity of bipolar disorder (BD) and OCD. More than half of patients with BD have an additional diagnosis, one of the most difficult to manage being OCD. More than 150 years ago, French psychiatrist Bénédict-Augustin Morel first described patients with BD-OCD, which resulted in questions regarding nosology and the clinical meaning of this condition.
In a standard 1969 psychiatry textbook, Mayer-Gross and colleagues,2 who had a significant focus on course of illness, included patients with BD-OCD in the manic-depressive disorders.2
In the hierarchical approach to diagnosis, which contradicts the DSM comorbidity approach, anxiety presentations like OCD should not be diagnosed as separate conditions when co-occurring with mood presentations such as BD. In other words, OCD should not be diagnosed unless BD is ruled out. If this non-DSM approach is correct, patients with OCD should be evaluated for family history for mood disorders, course of illness of mood symptoms in relation to OCD symptoms, and other evidence of bipolarity.
Unmet needs
BD-OCD comorbidity has importance in nosology as well as therapeutic implications. The question of nosology is whether this common comorbidity represents two separate diseases that co-occur by chance, or a severe subtype of BD or OCD. The therapeutic question is whether and how to treat the comorbidity since the main treatment for OCD serotonin reuptake inhibitors (SRIs) can worsen BD.
Although recent studies have looked at the co-occurrence of anxiety and bipolar disorders, there is insufficient research and the relationship between BD and OCD remains unclear. Given the available scientific evidence, however, some observations can be made (Table).
Comorbidity rates
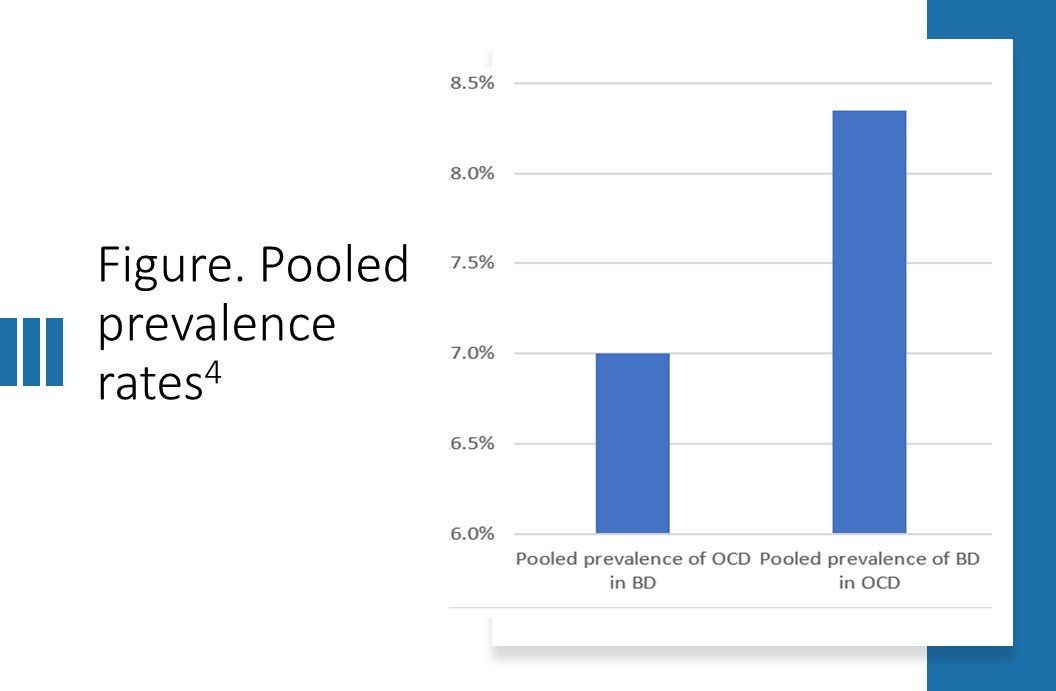
Apparent BD-OCD comorbidity is a common condition in psychiatry (Figure). Recent data from a large cross-continental multiple OCD treatment center study (3711 patients with OCD), showed a lifetime prevalence of comorbidity with BD-I and BD-II of 4.5% and 23.7%, respectively.3
In our meta-analysis, the pooled prevalence of OCD in BD was 17.0% (95% CI 12.7-22.4), which was comparable to the results reported by the pooled prevalence of BD in OCD (18.35%, 95% CI 13.2-24.8).4
Although limited by retrospective study design, small sample size, different thresholds for BD diagnosis (ie, categorical versus dimensional approach) and a different accuracy in diagnosing OCD (ie, discrimination between true ego-dystonic obsessions and depressive ruminations), these results confirm the relevance of comorbid BD-OCD.
Onset and course of illness
Most patients experience the onset of OCD before the onset of BD. Only in a few cases, the onset of OCD is concomitant with the first mood episode, rather than preceding or following it.5
As reported by recent studies, OC symptoms in childhood and adolescence seem to increase the risk of a later BD diagnosis, this being suggestive of partially shared etiopathogenetic mechanisms between these severe psychiatric disorders.6 Moreover, results from our meta-analysis showed higher comorbidity rates in youths (24.2%, 95% CI 10.36-41.60, n = 345, z = -9.5) compared with adults (13.56%, 95% CI 10.4-16.25, n = 539).7 Considering course of illness as a key diagnostic validator, especially among patients with a primary diagnosis of BD, most comorbid OCD cases appeared to be related to mood episodes. Obsessive compulsive symptoms in comorbid patients appeared more often-and sometimes exclusively-during depressive episodes, and comorbid BD and OCD cycled together, with obsessive compulsive symptoms often remitting during manic/hypomanic episodes.
Taken together, the evidence so far on BD-OCD nosology, supports the view that most comorbid OCD appears to be related to mood episodes. Obsessive compulsive symptoms in childhood and adolescence may be expression of vulnerability to BD and an increased risk for BD. Obsessive compulsive symptoms would initially coexist with BD symptoms, even cycling together, and would gradually tend to decrease in the adulthood.
Heredity
A few studies assessed family history for OCD or BD in comorbid BD-OCD probands using clinical interviews and clinical records. The majority of these studies reported a higher prevalence of family history for mood disorders and lower prevalence for OCD in patients with BD-OCD.8 Moreover, a family history for mood disorders was reported to be more frequent in episodic OCD patients than in continuous/chronic OCD patients.
Neurobiological correlates
Investigators from the US analyzed the serotonin-transporter (5-HTT) binding potential using positron-emission tomography (PET) and [11C]DASB, a radioligand with high sensitivity and specificity for 5-HTT. They reported higher 5-HTT binding potential in the insula, the posterior cingular cortex, the subgenual anterior cingulate cortex, and the dorsal cingulate cortex in patients with OCD-BD.9
From a neurobiological perspective, BD mostly showed hypoactivity in the orbitofrontal cortex (ie, decision making, impulse control) and in the dorsolateral prefrontal cortex (ie, planning, attentional set shifting) with grey matter volume reduction associated to manic episodes. OCD mainly presented hyperactivity of the orbitofrontal cortex with a deficit in emotional processing.10 The overlap of similar cortical-subcortical circuits may partially explain clinical features of comorbid BD-OCD during the course of illness.
Treatment strategies
If clinical observations are correct, then many patients who are said to have both BD and OCD in fact only have BD, with OCD symptoms being caused by or secondary to mood symptoms. Therefore, mood stabilization should be the primary goal in treating BD-OCD patients.11 The treatment implication would be that such patients would improve with mood stabilizers alone, for both mood and OCD symptoms.
Serotonin reuptake inhibitors would be unnecessary for OCD symptoms and, in fact, could undermine OCD treatment by worsening the underlying causal mood episodes. This worsening could occur in two ways: either by causing mania, which would trigger a mood cycle leading to later depression; or by causing a long-term worsening rapid-cycling course of illness, with more and more mood episodes, in turn producing more and more OCD symptoms. Adding SRIs may be needed only in a minority of patients who have BD with refractory OCD.11
Besides mood stabilizers, neuroleptics may also be effective in both BD and OCD. Aripiprazole augmentation to lithium carbonate, even at low doses (10-15 mg/d), seemed to be the best option in comorbid patients with treatment-resistance.11 Reports of exacerbation of OC symptoms with neuroleptic agents tend to relate to schizophrenia, not BD.12
Conclusions
Study findings suggest that most cases of DSM-based BD-OCD comorbidity are not in fact comorbidity as defined by Feinstein.1 Rather these are cases of BD, with OC symptoms as secondary manifestations of mood episodes. This observation does not deny the remaining patients who have two separate disorders, BD and OCD, that occur simultaneously.
Disclosures:
Dr Amerio is Researcher and Psychiatrist, Department of Neuroscience, Rehabilitation, Ophthalmology, Genetics, Maternal and Child Health (DINOGMI), Section of Psychiatry, University of Genoa, Genoa, Italy; IRCCS Ospedale Policlinico San Martino, Genoa, Italy; and Mood Disorders Program, Tufts Medical Center, Boston, MA. Dr Costanza is Chargée d'einsegment et de Recherche, Psychiatrist and Neurologist, Department of Psychiatry, Faculty of Medicine, University of Geneva (UNIGE), Geneva, Switzerland; Department of Psychiatry, ASO Santi Antonio e Biagio e Cesare Arrigo Hospital, Alessandria, Italy. Dr Aguglia is Researcher and Psychiatrist, DINOGMI, Section of Psychiatry, University of Genoa, and IRCCS Ospedale Policlinico San Martino; Dr Serafini is Associate Professor, DINOGMI, Section of Psychiatry, University of Genoa, and IRCCS Ospedale Policlinico San Martino. Dr Brakoulias is Conjoint Professor, School of Medicine, Western Sydney University, Blacktown Hospital, Sydney, NSW, Australia. Dr Amore is Professor, DINOGMI, Section of Psychiatry, University of Genoa, and IRCCS Ospedale Policlinico San Martino. Dr Ghaemi is Professor, Mood Disorders Program and Department of Psychiatry, Tufts University Medical School, Boston, MA. Drs Amerio, Costanza,Aguglia, Serafini, Brakoulias, and Amore report no conflicts of interest concerning the subject matter of this article; Dr Ghaemi reports that he is employed by Novartis Institutes for Biomedical Research and holds equity in Novartis.
References:
1. Maj M. Psychiatric comorbidity: an artefact of current diagnostic systems? Br J Psychiatry. 2005;186:182-184.
2. Mayer-Gross W, Slater E, Roth M. Clinical Psychiatry, 3rd ed. London: Elsevier Health Sciences; 1969.
3. Brakoulias V, Starcevic V, Belloch A, et al. Comorbidity, age of onset and suicidality in obsessive-compulsive disorder (OCD): an international collaboration. Compr Psychiatry. 2017;76:79-86.
4. Amerio A, Stubbs B, Odone A, et al. The prevalence and predictors of comorbid bipolar disorder and obsessive-compulsive disorder: a systematic review and meta-analysis. J Affect Disord. 2015;186:99-109.
5. Tonna M, Amerio A, Odone A, et al. Comorbid bipolar disorder and obsessive-compulsive disorder: which came first? Aust N Z J Psychiatry. 2016;50:695-698.
6. Cederlöf M, Lichtenstein P, Larsson H, et al. Obsessive-compulsive disorder, psychosis, and bipolarity: a longitudinal cohort and multigenerational family study. Schizophr Bull. 2015;41:1076-1083.
7. Amerio A, Odone A, Liapis CC, et al. Diagnostic validity of comorbid bipolar disorder and obsessive-compulsive disorder: a systematic review. Acta Psychiatr Scand. 2014;129:343-358.
8. Amerio A, Tonna M, Odone A, et al. Heredity in comorbid bipolar disorder and obsessive-compulsive disorder patients. Shanghai Arch Psychiatry. 2015;27:307-310.
9. Joshi G, Mick E, Wozniak J, et al. Impact of obsessive-compulsive disorder on the antimanic response to olanzapine therapy in youth with bipolar disorder. Bipolar Disord. 2010;12:196-204.
10. Ekman CJ, Lind J, Rydén E, et al. Manic episodes are associated with grey matter volume reduction - a voxel-based morphometry brain analysis. Acta Psychiatr Scand. 2010;122:507-515.
11. Amerio A, Maina G, Ghaemi SN. Updates in treating comorbid bipolar disorder and obsessive-compulsive disorder: a systematic review. J Affect Disord. 2019;256:433-440.
12. Fonseka TM, Richter MA, Müller DJ. Second generation antipsychotic-induced obsessive-compulsive symptoms in schizophrenia: a review of the experimental literature. Curr Psychiatry Rep. 2014;16:510.
Newsletter
Receive trusted psychiatric news, expert analysis, and clinical insights — subscribe today to support your practice and your patients.