CME
Article
Psychiatric Times
Substance Use Among Adolescents and Young Adults
Author(s):
In this CME, check out best practices for screening and treating adolescents and young adults with substance use issues.
Halfpoint/AdobeStock

CATEGORY 1 CME
Premiere Date: May 20, 2023
Expiration Date: November 20, 2024
This activity offers CE credits for:
1. Physicians (CME)
2. Other
All other clinicians either will receive a CME Attendance Certificate or may choose any of the types of CE credit being offered.
ACTIVITY GOAL
The goal of this activity is to recognize substance use disorders among adolescents and young adults, as well as learn strategies for treatment.
LEARNING OBJECTIVES
1. Understand the general epidemiology of substance use and substance use disorders among adolescents and young adults.
2. Understand best practices for screening and treating adolescents and young adults with substance use issues.
TARGET AUDIENCE
This accredited continuing education (CE) activity is intended for psychiatrists, psychologists, primary care physicians, physician assistants, nurse practitioners, and other health care professionals seeking to improve the care of patients with mental health disorders.
ACCREDITATION/CREDIT DESIGNATION/FINANCIAL SUPPORT
This activity has been planned and implemented in accordance with the accreditation requirements and policies of the Accreditation Council for Continuing Medical Education (ACCME) through the joint providership of Physicians’ Education Resource®, LLC, and Psychiatric Times®. Physicians’ Education Resource®, LLC, is accredited by the ACCME to provide continuing medical education for physicians.
Physicians’ Education Resource, LLC, designates this enduring material for a maximum of 1.5 AMA PRA Category 1 Credits™. Physicians should claim only the credit commensurate with the extent of their participation in the activity.
This activity is funded entirely by Physicians’ Education Resource, LLC. No commercial support was received.
OFF-LABEL DISCLOSURE/DISCLAIMER
This accredited CE activity may or may not discuss investigational, unapproved, or off-label use of drugs. Participants are advised to consult prescribing information for any products discussed. The information provided in this accredited CE activity is for continuing medical education purposes only and is not meant to substitute for the independent clinical judgment of a physician relative to diagnostic or treatment options for a specific patient’s medical condition. The opinions expressed in the content are solely those of the individual faculty members and do not reflect those of Physicians’ Education Resource, LLC.
FACULTY, STAFF, AND PLANNERS’ DISCLOSURES AND CONFLICT OF INTEREST (COI) MITIGATION
None of the staff of Physicians’ Education Resource, LLC, or Psychiatric Times or the planners of this educational activity have relevant financial relationship(s) to disclose with ineligible companies whose primary business is producing, marketing, selling, reselling, or distributing health care products used by or on patients. Dr Quiggle reports nothing to disclose regarding this article. Dr Burke reports he receives the following grant: NIDA/AACAP K12, Grant # 3K12DA000357-22S1. Dr Wilens reports he is a coeditor for Elsevier Psychiatric Clinics of North America (ADHD). Additionally, he receives grant/research support from the NIH (NIDA). He receives royalties for intellectual property from Cambridge University Press, Guilford Press, and Ironshore. Dr Wilens also works as a clinical consultant for Bay Cove Human Services, the Gavin Foundation, US Minor/Major League Baseball, the US National Football League, and White Rhino/3D.
For content-related questions, email us at PTEditor@mmhgroup.com. For questions concerning the accreditation of this CE activity or how to claim credit, please contact info@gotoper.com and include “Substance Use Among Adolescents and Young Adults” in the subject line.
HOW TO CLAIM CREDIT
Once you have read the article, please use the following URL to evaluate and request credit: https://education.gotoper.com/activity/ptcme23may. If you do not already have an account with Physicians’ Education Resource, LLC, you will be prompted to create one. You must have an account to evaluate and request credit for this activity.
Adolescence is a developmental stage characterized by rapid physical and psychosocial growth and maturation.1 With such dynamic neurobiological and social changes come a unique set of vulnerabilities to risk taking and substance use. Limbic reward-mediated pathways develop prior to the maturation of executive control centers in the prefrontal cortex and may offer a neurobiological explanation for the propensity toward risk-taking behaviors among adolescents.2
As compared to other age demographics, adolescents have the greatest access to substances coupled with the lowest perception of substance-associated risks.3 This is a critical point, as perception of the harm a substance may pose is generally inversely related to its use in adolescents and young individuals. By the senior year of high school, more than 61% of students report having tried alcohol, 41% have experimented with illicit drugs, and nearly 10% have used a prescription medication nonmedically.4 In a recent study evaluating the history of cannabis use, adolescents were twice as likely to develop a cannabis use disorder (CUD) compared to their young adult counterparts.5 Furthermore, increasing frequency of use is associated with incrementally higher risk of developing a CUD.
According to the 2021 National Survey on Drug Use and Heath, nearly 10% of youth aged 12 to 17 met criteria for a substance use disorder (SUD), and young adults aged 18 to 25 were the most likely of any age group to have an SUD (> 25%).3 Despite research showing that half of all SUDs manifest in adolescence (and approximately 80% develop by age 25), adolescents and young adults are the least likely of any age group to obtain treatment.6 In the past decades, with the emergence of synthetic opioids such as fentanyl on the illicit drug market, annual rates of both opioid use disorder (OUD) diagnoses and unintentional overdoses have risen among adolescents and young adults. Nevertheless, approximately 75% of adolescents and young adults were not prescribed an FDA-approved medication for their OUD.7 Recent data on the dispensing of buprenorphine between 2015 and 2020 is concerning. Although the dispensing of buprenorphine has increased significantly for individuals 20 years of age or older, it has decreased by 45% for youth under the age of 20.8
Impacts of Substance Use
Substance use is a major cause of disability among adolescents and young adults globally.9 Substance use has been shown to have a multitude of developmental impacts across the psychosocial, neuropsychological, and physical domains. Impaired familial relationships, lower educational attainment, higher rates of unemployment, and lower reports of overall life satisfaction have been found among adolescents and young adults who use substances, even after correcting for multiple potential confounders.10
Although some neuropsychological features may increase the underlying risk of substance use in adolescents (eg, deficits in inhibitory executive function control), longitudinal studies suggest that cannabis use is associated with worse performance on tests of attention and memory, lower processing speeds,11 as well as potential long-term deficits in executive functioning and verbal IQ even after cessation of use.12 Short-term cognitive effects of cannabis can last up to 8 hours and highlight concerns about driving under the influence. The risk of involvement in a motor vehicle accident increases 2-fold after recent cannabis use.13 Structural and functional neuroimaging studies have likewise found an association between heavy alcohol use in adolescence to changes in gray and white matter volumes and increased brain activation during tasks of inhibition and working memory, compared with controls.11
Adolescent-onset SUDs have also been shown to predict all-cause mortality in young adulthood and are associated with infectious diseases such as HIV and hepatitis C, risky sexual behaviors, motor vehicle accidents, drug trafficking, and suicide attempts.14
Screening and Evaluation
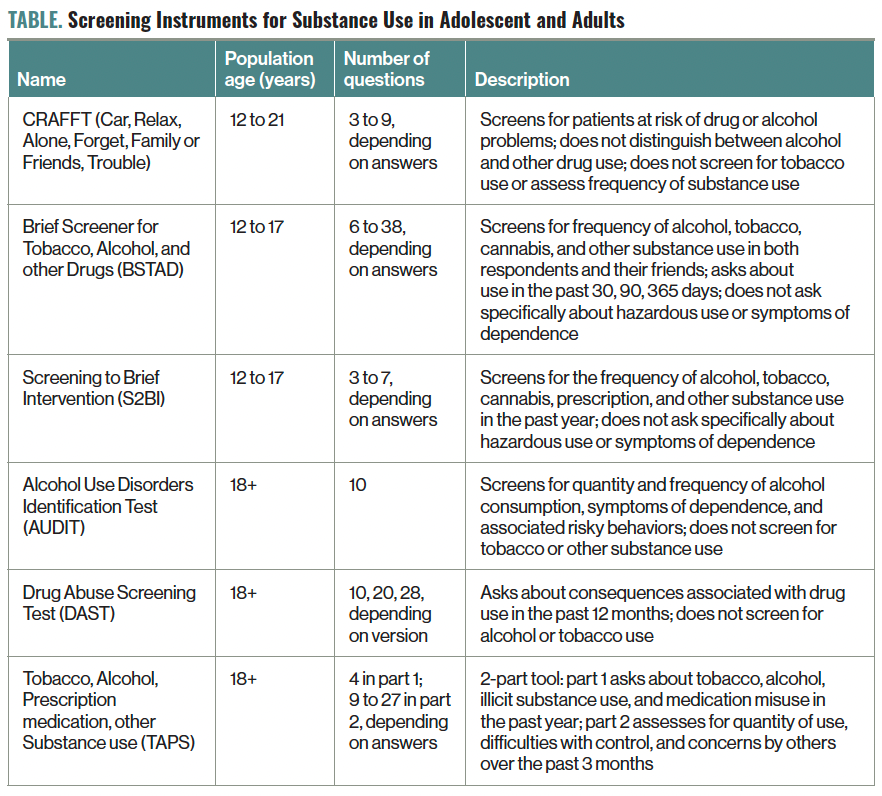
Given the high rates of substance use and associated morbidity among adolescents and young adults, adequate screening and referral is of paramount importance. The American Academy of Pediatrics (AAP) recommends universal screening, brief intervention, and referral to treatment (SBIRT) in the primary care setting.15 Several validated screening instruments (free and available online) can be used across a range of clinical settings and are outlined in the Table. The CRAFFT (Car, Relax, Alone, Forget, Family or Friends, Trouble); Brief Screener for Tobacco, Alcohol, and other Drugs (BSTAD); and Screening to Brief Intervention (S2BI) are commonly used tools to screen adolescents and young adults. Other instruments, such as the Alcohol Use Disorders Identification Test (AUDIT); Drug Abuse Screening Test (DAST); and Tobacco, Alcohol, Prescription medication, other Substance use (TAPS) tool have been validated for use in adult populations and are being used variably in adolescents. Some of these instruments are available in electronic medical records and can be administered via patient-related outcome measures through tablets and/or internet portals.
Table. Screening Instruments for Substance Use in Adolescent and Adults
Because more than 75% of adolescents with an SUD have a comorbid mental health diagnosis, any comprehensive evaluation should include careful attention to the assessment of common psychiatric comorbidities, including disorders of conduct, mood, anxiety, and attention-deficit/hyperactivity disorder.16 Important considerations with respect to a substance use history include age at first use, pattern of use, time of last use, route of use, history of withdrawal, consequences to use, temporal correlation between use and other psychiatric symptoms, and associated risky behaviors. Objective data such as urine or oral fluid (saliva) drug screens, serum phosphatidylethanol (PEth) tests, and quantitative cannabis levels can provide important baseline markers and can be useful for monitoring treatment response over time.
The DSM-5 can aide in the diagnosis of an SUD.17 In order to make a diagnosis, one must establish a history of problematic use leading to clinically significant impairment or distress over a 12-month period. At least 2 of 11 criteria, generally involving impaired control, social impairment, risky use, and physiologic dependence, must be met. SUDs can be conceptualized on a spectrum of severity: mild (2-3 criteria), moderate (4-5 criteria), and severe (6 or more criteria). While the diagnostic criteria to establish an SUD are the same for adolescents and adults, diagnostic challenges can arise from the discordance between patient and parent report. Special attention to functional impairment as evidenced by declining grades, changes in friend groups, social problems, and risky behaviors can be helpful in making a diagnosis.
Treatment
An integrated, multipronged approach that pays particular attention to the developmental stage of the patient is recommended for the treatment of adolescents and young adults with SUDs. Motivational interviewing, a communicative strategy that attempts to elicit a patient’s intrinsic motivation for change by resolving ambivalence, can be a useful framework for engaging and working with this patient population.18 In addition, motivational enhancement therapy, Adolescent Community Reinforcement Approach (A-CRA), cognitive behavioral therapy (CBT), contingency management, and a variety of family-based therapies are all considered effective behavioral interventions for youth.19 The Community Reinforcement and Family Training (CRAFT) model can provide family members with helpful evidence-based tools that teach strategies targeting motivation and behavior change, positive communication, and self-care.20 Given both the vulnerabilities to substance use and lack of treatment engagement in the adolescent population, low-threshold treatment models that are flexible to the developmental needs of this population have emerged.21
Evidence-based psychopharmacologic treatments for core symptoms of SUD in adolescents and young adults are limited. For OUD, only buprenorphine is FDA approved for patients under the age of 18 (16 years of age and older); methadone and long-acting naltrexone are approved in adult patients. Although there are no FDA approved medications for alcohol use disorder in patients under the age of 18, there is evidence for the use of naltrexone as an off-label treatment in this population.22 In the treatment of CUD, a randomized controlled trial (RCT) has shown benefit for n-acetylcysteine (NAC) in study participants aged 15 to 21.23 Of note, a similarly designed study looking at NAC for CUD in patients 18 to 50 years of age showed post hoc that study participants aged 18 to 21 years demonstrated an effect size of a similar magnitude as found in the adolescent study.24 Given these limited treatment options, there is an urgent need for further evaluation of the safety and efficacy of novel therapeutics for SUDs in young individuals.
Data are mixed on how the treatment of co-occurring psychiatric disorders impact substance use. For example, in mood disorders, in a small RCT looking at adolescents with underlying bipolar disorder, the use of lithium resulted in decreased substance use and overall improvements in levels of functioning25; whereas another recent pilot study with quetiapine in bipolar youth showed improved mood without changes in SUD.26 In contrast, in a population of adolescents with major depression, substance use, and behavioral problems, combined treatment with an SSRI and CBT showed variable improvements in depressive symptoms, but did not affect self-reported substance use outcomes.27 In part, this was related to the concomitant CBT being administered in both groups. Given these nonoverlapping treatment outcomes, tailored treatment plans should address both the SUD as well as the co-occurring psychiatric disorder, particularly if the patient has severe mood instability and/or psychosis.
Concluding Thoughts
Overall, substance use in adolescents and young adults remains a serious public health concern and poses a unique set of risks to the developing brain. Further efforts are needed to screen for SUDs and engage this vulnerable population in treatment.
Dr Quiggle is an addiction psychiatry fellow at Mass General Brigham. Dr Burke is a psychiatrist in Boston, Massachusetts and is affiliated with multiple hospitals in the area, including Massachusetts General Hospital and McLean Hospital. Dr Wilens is chief of the Division of Child and Adolescent Psychiatry and is codirector of the Center for Addiction Medicine at Massachusetts General Hospital.
References
1. Chulani VL, Gordon LP. Adolescent growth and development. Prim Care. 2014;41(3):465-487.
2. Casey BJ, Jones RM. Neurobiology of the adolescent brain and behavior: implications for substance use disorders. J Am Acad Child Adolesc Psychiatry. 2010;49(12):1189-1201.
3. Key substance use and mental health indicators in the United States: results from the 2021 National Survey on Drug Use and Health. Substance Abuse and Mental Health Services Administration. December 2022. Accessed April 3, 2023. https://www.samhsa.gov/data/sites/default/files/reports/rpt39443/2021NSDUHFFRRev010323.pdf
4. Johnston LD, Miech RA, Patrick ME, et al. Monitoring the future: national survey results on drug use, 1975–2022. Institute for Social Research, The University of Michigan. 2023. Accessed April 3, 2023. https://monitoringthefuture.org/wp-content/uploads/2023/01/mtfoverview2022.pdf
5. Volkow ND, Han B, Einstein EB, Compton WM. Prevalence of substance use disorders by time since first substance use among young people in the US. JAMA Pediatr. 2021;175(6):640-643.
6. Compton WM, Thomas YF, Stinson FS, Grant BF. Prevalence, correlates, disability, and comorbidity of DSM-IV drug abuse and dependence in the United States. Arch Gen Psychiatry. 2007;64(5):566-576.
7. Hadland SE, Wharam JF, Schuster MA, et al. Trends in receipt of buprenorphine and naltrexone for opioid use disorder among adolescents and young adults, 2001-2014. JAMA Pediatr. 2017;171(8):747-755.
8. Terranella A, Guy GP, Mikosz C. Buprenorphine dispensing among youth aged ≤19 years in the United States: 2015–2020. Pediatrics. 2023;151(2):e2022058755.
9. Erskine HE, Moffitt TE, Copeland WE, et al. A heavy burden on young minds: the global burden of mental and substance use disorders in children and youth. Psychol Med. 2015;45(7):1551-1563.
10. Stormshak EA, DeGarmo DS, Chronister KM, et al. The impact of substance use during middle school and young adulthood on parent–young adult relationships. J Fam Psychol. 2019;33(7):797-808.
11. Squeglia LM, Gray KM. Alcohol and drug use and the developing brain. Curr Psychiatry Rep. 2016;18(5):46.
12. Castellanos-Ryan N, Pingault JB, Parent S, et al. Adolescent cannabis use, change in neurocognitive function, and high-school graduation: a longitudinal study from early adolescence to young adulthood. Dev Psychopathol. 2017;29(4):1253-1266.
13. Hartman RL, Huestis MA. Cannabis effects on driving skills. Clin Chem. 2013;59(3):478-492.
14. Clark DB, Martin CS, Cornelius JR. Adolescent-onset substance use disorders predict young adult mortality. J Adolesc Health. 2008;42(6):637-639.
15. Levy SJL, Kokotailo PK; Committee on Substance Abuse. Substance use screening, brief intervention, and referral to treatment for pediatricians. Pediatrics. 2011;128(5):e1330-e1340.
16. Garofoli M. Adolescent substance abuse. Prim Care. 2020;47(2):383-394.
17. Diagnostic and statistical manual of mental disorders, Fifth Edition. American Psychiatric Association Publishing; 2013.
18. Jensen CD, Cushing CC, Aylward BS, et al. Effectiveness of motivational interviewing interventions for adolescent substance use behavior change: a meta-analytic review. J Consult Clin Psychol. 2011;79(4):433-440.
19. Adams ZW, Marriott BR, Hulvershorn LA, Hinckley J. Treatment of adolescent cannabis use disorders. Child Adolesc Psychiatr Clin N Am. 2023;32(1):141-155.
20. Kirby KC, Versek B, Kerwin ME, et al. Developing Community Reinforcement and Family Training (CRAFT) for parents of treatment-resistant adolescents. J Child Adolesc Subst Abuse. 2015;24(3):155-165.
21. Wilens TE, McKowen J, Kane M. Transitional-aged youth and substance use: teenaged addicts come of age. Contemp Pediatr. November 1, 2013. Accessed April 3, 2023. https://www.contemporarypediatrics.com/view/transitional-aged-youth-and-substance-use-teenaged-addicts-come-age
22. Miranda R, Ray L, Blanchard A, et al. Effects of naltrexone on adolescent alcohol cue reactivity and sensitivity: an initial randomized trial. Addict Biol. 2014;19(5):941-954.
23. Gray KM, Carpenter MJ, Baker NL, et al. A double-blind randomized controlled trial of n-acetylcysteine in cannabis-dependent adolescents. Am J Psychiatry. 2012;169(8):805-812.
24. Gray KM, Sonne SC, McClure EA, et al. A randomized placebo-controlled trial of N-acetylcysteine for cannabis use disorder in adults. Drug Alcohol Depend. 2017;177:249-257.
25. Geller B, Cooper TB, Sun K, et al. Double-blind and placebo-controlled study of lithium for adolescent bipolar disorders with secondary substance dependency. J Am Acad Child Adolesc Psychiatry. 1998;37(2):171-178.
26. Yule AM, DiSalvo M, Kramer J, et al. A pilot, randomized controlled trial of quetiapine for youth with co-occuring substance use disorder and bipolar disorder. J Am Acad Child Adolesc Psychiatry. 2022;61(10):S271.
27. Riggs PD, Mikulich-Gilbertson SK, Davies RD, et al. A randomized controlled trial of fluoxetine and cognitive behavioral therapy in adolescents with major depression, behavior problems, and substance use disorders. Arch Pediatr Adolesc Med. 2007;161(11):1026-1034.

Newsletter
Receive trusted psychiatric news, expert analysis, and clinical insights — subscribe today to support your practice and your patients.






