News
Article
Psychiatric Times
The Making of Adult ADHD: The Rapid Rise of a Novel Psychiatric Diagnosis
"The history of psychiatry is a history of fads in theory, diagnosis, and treatment. Such rapid shifts in conceptualization—such as the emergence of the concept of adult ADHD—almost always warrant informed critical examination."
Joel bubble ben_AdobeStock

COMMENTARY
As recently as 2 decades ago, the consensus view in American academic psychiatry was that attention-deficit/hyperactivity disorder (ADHD) rarely, if ever, persists into adulthood.1,2 For decades, ADHD was considered a disorder of childhood; adult cases were seen uncommonly and the diagnosis was rarely made. DSM-IV-TR, published in 2000, describes a condition existing in children and makes only scant reference to adults.3
Fast-forward to 2023, and adult ADHD is the diagnosis du jour; rates of diagnosis are skyrocketing at an alarming rate as are prescriptions for psychostimulants, the drugs that purportedly treat the condition.
The history of psychiatry is a history of fads in theory, diagnosis, and treatment. Such rapid shifts in conceptualization—such as the emergence of the concept of adult ADHD—almost always warrant informed critical examination.
In the case of a novel psychiatric disorder, it is either true that (1) psychopathologists and psychiatric nosologists have missed the disorder for more than a century, or (2) that the disorder is a case of disease mongering, when a condition that has never been observed is suddenly made popular overnight as a result of social, cultural, and economic reasons. We argue that the latter is true for adult ADHD.
How did adult ADHD get its wheels? The rise in diagnosis of adult ADHD fully coincides with marketing by the pharmaceutical industry when Eli Lilly and Company got the first US Food and Drug Administration indication for this label with atomoxetine (Strattera) in 1996. Since that date, many academics have been promoting the concept of adult ADHD. The adult ADHD market has become a multibillion-dollar industry, with the rise of digital companies specializing in online diagnosis and treatment—some of which have come under legal scrutiny.
Does ADHD Persist Into Adulthood?
Findings from commonly cited retrospective studies suggest that approximately 50% to 60% of childhood ADHD persists into adulthood. These studies look backwards to attempt to determine which childhood cases continue into adulthood. However, these data are disproven by prospective studies, which repeatedly show that about 80% of children with ADHD do not continue to have that diagnosable condition, followed prospectively either into young adulthood or even for 33 years into their fourth decade of life (Figure).4,5
Figure. Children With ADHD Into Adulthood
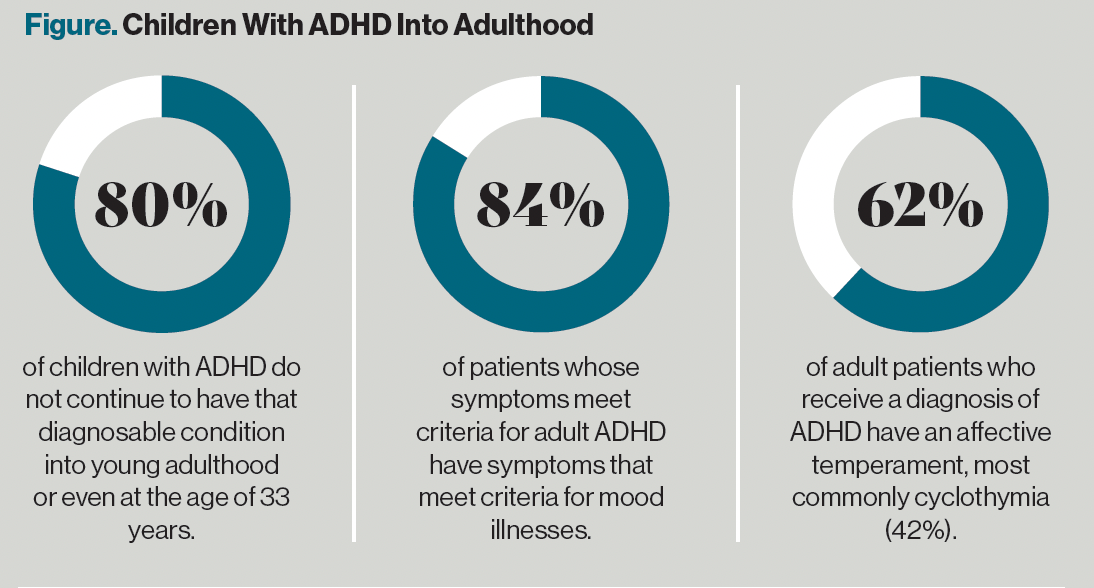
A total of 20% of cases persist, whereas 80% do not. In other words, most children with ADHD do not continue to meet the criteria for the diagnosis into adulthood. These data are reviewed more thoroughly at https://psychiatryletter.com/adult-add/.
Construct Validity and Diagnostic Hierarchy
When we argue that adult ADHD is not a scientifically valid diagnosis, we do not mean, of course, that the symptoms so attributed do not exist. Clearly, adult human beings can exhibit problems with attention, concentration, focus, memory, and related abilities.
What we mean is that these symptoms have not been shown to be the result of a scientifically valid disease (adult ADHD) and are better explained by more classic and scientifically validated psychiatric conditions, namely diseases or abnormalities of mood, anxiety, and mood temperament.
A major problem with the DSM system as currently constituted is that it fails to take into account the concept of diagnostic hierarchy, a fundamental diagnostic principle used across medicine. In sum, diagnostic hierarchy refers to the idea that not all diagnoses are created equal—that some are more important or more primary than others.
Failure to adhere to the concept of diagnostic hierarchy has resulted in epidemics of polydiagnosis (assigning multiple diagnoses to the same patient) and polypharmacy (the use of multiple psychiatric medications, often across classes).
What Causes the Symptoms Attributed to Adult ADHD?
Plenty of other psychiatric disorders exist that can cause ADHD-like symptoms, and in current practice, individuals with these symptoms receive misdiagnoses of adult ADHD.
For example, 84% of patients with symptoms meeting criteria for adult ADHD also have symptoms that meet criteria for mood illnesses.6 Using the concept of diagnostic hierarchy, poor attention is a symptom of depression, mania, and anxiety; thus, the occurrence of inattention while a patient has mood symptoms does not mean the patient has both an attention disorder and a mood disorder.
This would be like saying every person with pneumonia also has a fever disorder. It is common to find that someone who thinks they have adult ADHD has another illness, such as a mood or anxiety condition, that causes the symptom of inattention.
Another underappreciated consideration is the concept of mood temperament. Unlike the symptoms of major mood disorders, mood temperaments do not come and go; they are present all the time as part of one’s personality.
Conditions such as cyclothymia, hyperthymia, and dysthymia involve constant presence of mild manic and/or depressive symptoms. Since these manic and/or depressive symptoms are present all the time, they can produce inattention, poor concentration, and poor executive function all the time.
One of us (NG) recently published with colleagues the first study on the topic of misdiagnosis of mood temperament on ADHD.7 We found that 62% of patients who received a diagnosis of adult ADHD actually have an affective temperament, most commonly cyclothymia (42%). In patients treated with amphetamine, mood symptoms predictably worsened.
Why Do the Drugs Work?
A common claim is that since psychostimulants improve the cognition of individuals diagnosed with adult ADHD, then they must be treating an underlying disorder. But this is faulty logic. Psychostimulants improve cognition for everyone, including normal patients without psychiatric illness. It is because they have this general effect that they are so widely abused; it says nothing about the existence of adult ADHD.
Concluding Thoughts
The history of psychiatry teaches us that the field has been vulnerable to a host of diagnostic fads. Adult ADHD is the latest of such fads, and a careful review of the scientific literature reveals that the range of ADHD-like symptoms in adults is more accurately explained by other empirically validated psychiatric disorders. This has significant ramifications for therapy, given the wide use of psychostimulants in the treatment of these patients.
The opinions expressed are those of the authors and do not necessarily reflect the opinions of Psychiatric Times.
Dr Ruffalo is an instructor of psychiatry at the University of Central Florida College of Medicine in Orlando and adjunct instructor of psychiatry at Tufts University School of Medicine in Boston, Massachusetts. Dr Ghaemi is director of the Psychopharmacology Consultation Clinic at Tufts Medical Center and a professor of psychiatry at Tufts University School of Medicine.
References
1. Shorter E. The Rise and Fall of the Age of Psychopharmacology. Oxford University Press; 2021.
2. Tayag Y. Adult ADHD is the wild west of psychiatry. Atlantic. April 14, 2023. Accessed August 3, 2023. https://www.theatlantic.com/health/archive/2023/04/adult-adhd-diagnosis-treatment-adderall-shortage/673719/
3. American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders. 4th ed. American Psychiatric Publishing; 2000.
4. Caye A, Rocha TBM, Anselmi L, et al. Attention-deficit/hyperactivity disorder trajectories from childhood to young adulthood: evidence from a birth cohort supporting a late-onset syndrome. JAMA Psychiatry. 2016;73(7):705-712.
5. Klein RG, Mannuzza S, Olazagasti MAR, et al. Clinical and functional outcome of childhood attention-deficit/hyperactivity disorder 33 years later. Arch Gen Psychiatry. 2012;69(12):1295-1303.
6. Kessler RC, Adler L, Barkley R, et al. The prevalence and correlates of adult ADHD in the United States: results from the National Comorbidity Survey Replication. Am J Psychiatry. 2006;163(4):716-723.
7. Mauer S, Ghazarian G, Ghaemi SN. Affective temperaments misdiagnosed as adult attention deficit disorder: prevalence and treatment effects. J Nerv Ment Dis. 2023;211(7):504-509.

Newsletter
Receive trusted psychiatric news, expert analysis, and clinical insights — subscribe today to support your practice and your patients.






