Publication
Article
Psychiatric Times
Adolescent Substance Use: Reasons for Optimism and Concern
Author(s):
"Although adolescent substance use is a topic that can be challenging for families and clinicians alike, data demonstrate that interventions during this time are effective for preventing, identifying, and reducing risky use."
Joshua Resnick_AdobeStock

There are reasons to be optimistic about adolescent substance use given an overall consistent decline in use for this age group over the past 20 years. However, nicotine and cannabis use have fluctuated, and adolescents have been disproportionately impacted by the development of electronic vaping devices.
Likewise, adolescents have been disproportionately affected by the increase in counterfeit pills containing illicitly manufactured fentanyl, and there has recently been a sharp increase in drug overdose deaths.
For these reasons, it is important that child and adolescent behavioral health clinicians remain vigilant regarding early identification of substance use, as youth with mental health conditions who use substances are at increased risk for developing a substance use disorder (SUD).
Prevalence
Adolescent substance use is tracked annually in the United States by several surveys. The Monitoring the Future (MTF) study, for example, has collected self-reported information from 12th graders since 1975. The most commonly used substances by adolescents across surveys include alcohol, cannabis, and nicotine. There has been a general overall decline in substance use among adolescents over the past 20 years, with a notable decline across all substances when stricter COVID-19 pandemic restrictions were in place during 2020-2021.1
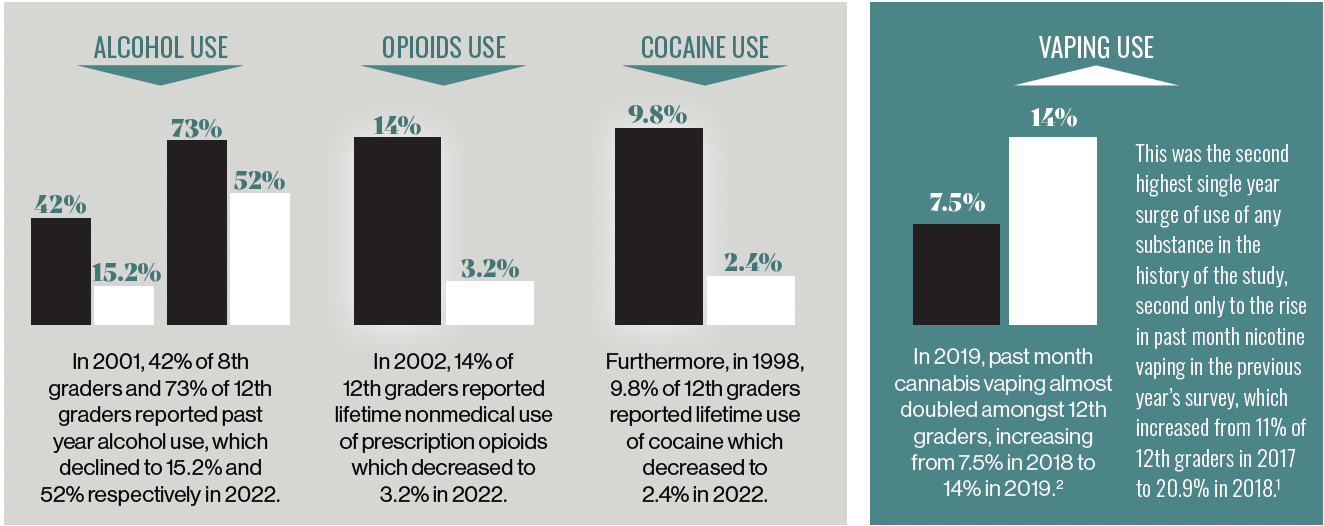
Overall declines in substance use among adolescents are reflected in the MTF study in the prevalence of use for substances including alcohol, opioids, and cocaine.1 In 2001, 42% of 8th graders and 73% of 12th graders reported past year alcohol use, which declined to 15.2% and 52% respectively in 2022. In 2002, 14% of 12th graders reported lifetime nonmedical use of prescription opioids, which decreased to 3.2% in 2022. Furthermore, in 1998, 9.8% of 12th graders reported lifetime use of cocaine, which decreased to 2.4% in 2022.
In contrast with other substances, sharp increases in the use of nicotine and cannabis with an electronic vaping device have been a concern. In 2019, past month cannabis vaping had almost doubled among 12th graders in the MTF study, increasing from 7.5% in 2018 to 14% in 2019.2
This was the second highest single-year surge in the use of any substance in the history of the study, second only to the rise in past month nicotine vaping in the previous year’s survey, which had increased from 11% of 12th graders in 2017 to 20.9% in 2018.1
Nicotine and Cannabis Vaping
Nicotine vaping among adolescents is concerning due to the risk for nicotine addiction. It is estimated that only 5 mg of nicotine per day (the equivalent of 5 standard cigarettes) can lead to the development of nicotine dependence in young individuals. The pods for one popular vaping device, JUUL, contain approximately 41.3 mg of nicotine, the equivalent of about 2 packs of cigarettes.3
Although individuals who smoke cigarettes can easily track their use in packs per day, it is more difficult to quantify the amount of nicotine being consumed through vaping.
Additionally, adolescents perceive vaping to have insignificant risk and view it as safer than cigarette use, despite the lack of evidence for this assumption. In addition to addiction risk, the vapor from e-cigarettes contains chemicals with known toxicity, including nicotine, lead, heavy metals, and carcinogens.
Vaping cannabis (liquid or oil concentrates) instead of using other cannabis products, such as the plant, is more common among adolescents than other age groups in part because it is easier for adolescents to conceal their use.
There is particular concern regarding adolescent cannabis vaping because the concentrates used typically have a much higher tetrahydrocannabinol (THC) concentration (25% to 90% THC) relative to the cannabis plant (12% to 16% THC). The risk of adverse events associated with cannabis use, such as acute anxiety or paranoia, increases with greater cannabis concentration.4
Furthermore, there is little regulation of cannabis concentrates. Between 2019 and 2020, a sharp increase occurred in hospitalizations for respiratory symptoms linked to the use of vaping products. Adolescents accounted for 15% of 2700 hospitalizations during this period. The Centers for Disease Control and Prevention identified a chemical added to some THC-containing vape fluids—vitamin E acetate—as the likely cause, although other chemicals may have also contributed.5
The legal and medical landscape around cannabis adds to confusion about its safety and potential benefits. With increased legalization of “medical marijuana,” there are misconceptions that THC products may be therapeutic for some psychiatric conditions.
However, there have yet to be studies whose findings demonstrate the clear efficacy of cannabis for the treatment of such indications, whereas clear data exist supporting the deleterious effects of regular cannabis use on the developing brain.6
Despite this, an ever-increasing number of products are entering the market, at recreational or medical dispensaries, before adequate studies can be done to ascertain the safety of these products.
Illicitly Manufactured Fentanyl
Illicitly manufactured fentanyl has driven the rise in adult drug overdose deaths in the United States for the past decade, as it has increasingly been found to infiltrate or even replace the heroin supply. Although heroin use among adolescents is relatively rare, adolescents are being exposed to fentanyl through counterfeit pressed pills.
This is particularly concerning because fentanyl exposure drove a 109% increase in adolescent drug overdose deaths between 2019 and 2021.7 Among the 2231 adolescent deaths during this time frame, 84% involved illicitly manufactured fentanyl, and counterfeit pills were present in 25% of deaths.
Unfortunately, counterfeit pills are easily accessible to adolescents and young adults, particularly through social media apps. In most cases, adolescents are not aware that the substance they are using contains fentanyl, and instead think they are taking other substances, such as prescription stimulants and benzodiazepines or recreational drugs such as ecstasy or other “club drugs.” Unfortunately, because of the lethality of fentanyl, particularly in naïve users, a single dose can be fatal.
Mental Health Comorbidities
When considering substance use patterns, it is important to remember that some adolescents are more vulnerable to developing an SUD. SUD risk is multifactorial, and risks include family history of an SUD, type of substance used, and comorbidity.
For example, approximately 50% of an individual’s risk for developing an SUD is heritable.8 Because SUD is highly stigmatized, families may struggle to discuss this history, but it is valuable information for adolescents to know when considering their own risks. Furthermore, some substances, such as nicotine and cocaine, are more addictive than others.9
Lastly, childhood-onset psychiatric disorders are also associated with increased risk for developing an SUD. For example, attention-deficit/hyperactivity disorder, depression, conduct disorder, and posttraumatic stress disorder are associated with a 2 to 5 times greater risk for developing an SUD.10,11
The Behavioral Health Clinician
Despite the known consequences of early problematic substance use, access to adequate treatment is lacking, and behavioral health clinicians can play an important role in the identification and treatment of problematic substance use. Unfortunately, the stigma associated with addiction can be a barrier to discussing substance use for adolescents, families, and clinicians.
Behavioral health clinicians who treat children, adolescents, and young adults should be having nonjudgmental discussions about substance use as part of every psychiatric evaluation. Clinicians are also an important source of information regarding the risks of substance use on the developing brain. They can help clarify confusing or incorrect information that patients and families may have.
For adolescents who meet criteria for an SUD, treatment in the form of medication may be indicated, particularly for opioid use disorders. Regrettably, although the rate of overdose deaths in adolescents has skyrocketed, rates of buprenorphine dispensed to patients aged 19 years or younger decreased by 25% between 2015 and 2020.12
Rates of prescribing to adults increased by 47% in the same time frame, suggesting specific barriers for adolescents in obtaining treatment with this medication, which is approved by the US Food and Drug Administration for patients 16 years and older for the treatment of opioid use disorder.
As prescribing barriers for buprenorphine decrease with the removal of the X-waiver requirement, special attention should be paid to increasing awareness of and comfort with this medication among physicians treating adolescents.
In addition, increased access to the overdose reversal agent, naloxone, and public health efforts to educate youth, families, and schools on its use will be crucial to combat deaths in those who may not meet the criteria for an addictive disorder but who may encounter a lethal dose of fentanyl through unwitting use of counterfeit pressed pills.
Concluding Thoughts
Although adolescent substance use is a topic that can be challenging for families and clinicians alike, data demonstrate that interventions during this time are effective for preventing, identifying, and reducing risky use. As with other sensitive topics in mental health, an open, honest, and nonjudgmental approach goes a long way in establishing the necessary rapport to address these issues.
Given the frequent comorbidity of substance use with other mental health conditions, as well as the risk of exacerbation of psychiatric symptoms that substance use poses, clinicians who work with adolescents and young adults should become comfortable with evaluating and treating SUDs in this population.
Dr Creedon is an assistant professor of clinical psychiatry at Louisiana State University Health Sciences Center New Orleans. Dr Abdurakhmanov is a psychiatry resident at Louisiana State University in Shreveport. Dr Yule is vice chair of addiction psychiatry at Boston Medical Center, Boston University Chobanian & Avedisian School of Medicine in Massachusetts.
References
1. Miech RA, Johnston LD, Patrick ME, et al. Monitoring the Future: National Survey Results on Drug Use, 1975-2022: Secondary School Students. Institute for Social Research, The University of Michigan; 2023. Accessed March 23, 2023. https://monitoringthefuture.org/wp-content/uploads/2022/12/mtf2022.pdf
2. Miech RA, Patrick ME, O’Malley PM, et al. Trends in reported marijuana vaping among US adolescents, 2017-2019. JAMA. 2020;323(5):475-476.
3. Pierce JP, Zhang J, Crotty Alexander LE, et al. Daily e-cigarette use and the surge in JUUL sales: 2017-2019. Pediatrics. 2022;149(6):e2021055379.
4. PRSC Cannabis Concentration Workgroup. Cannabis concentration and health risks: a report for the Washington State Prevention Research Subcommittee (PRSC). University of Washington. November 2020. Accessed March 23, 2023. https://adai.uw.edu/wordpress/wp-content/uploads/2020/11/Cannabis-Concentration-and-Health-Risks-2020.pdf
5. Krishnasamy VP, Hallowell BD, Ko JY, et al; Lung Injury Response Epidemiology/Surveillance Task Force. Update: characteristics of a nationwide outbreak of e-cigarette, or vaping, product use–associated lung injury — United States, August 2019–January 2020. MMWR Morb Mortal Wkly Rep. 2020;69(3):90-94.
6. Hill KP, Gold MS, Nemeroff CB, et al. Risks and benefits of cannabis and cannabinoids in psychiatry. Am J Psychiatry. 2022;179(2):98-109.
7. Tanz LJ, Dinwiddie AT, Mattson CL, et al. Drug overdose deaths among persons aged 10-19 Years - United States, July 2019-December 2021. MMWR Morb Mortal Wkly Rep. 2022;71(50):1576-1582.
8. Bevilacqua L, Goldman D. Genes and addictions. Clin Pharmacol Ther. 2009;85(4):359-361.
9. Tsuang MT, Lyons MJ, Harley RM, et al. Genetic and environmental influences on transitions in drug use. Behav Genet. 1999;29(6):473-479.
10. Groenman AP, Janssen TWP, Oosterlaan J. Childhood psychiatric disorders as risk factor for subsequent substance abuse: a meta-analysis. J Am Acad Child Adolesc Psychiatry. 2017;56(7):556-569.
11. Lopez B, Turner RJ, Saavedra LM. Anxiety and risk for substance dependence among late adolescents/young adults. J Anxiety Disord. 2005;19(3):275-294.
12. Terranella A, Guy GP Jr, Mikosz C. Buprenorphine dispensing among youth aged ≤19 years in the United States: 2015–2020. Pediatrics. 2023;151(2):e2022058755.

Newsletter
Receive trusted psychiatric news, expert analysis, and clinical insights — subscribe today to support your practice and your patients.






