Publication
Article
Psychiatric Times
Unique Collaborative Care System: Solution to the Youth Mental Health Crisis
Author(s):
Integrated models of care offer real time solutions by enabling primary care to identify and address behavioral health concerns through routine screening and early intervention more efficiently. Learn more here.
premyuda/AdobeStock

The beginning of our story is not unique. Two of us—Ben Hillyard, MEd, LCMHC, and Jessica Lyons, MS, LMFT—spent decades working in the broken mental health system, alarmed by access-to-care challenges, emergency department (ED) boarding of patients, and the rapidly growing youth mental health crisis. Together, we shared a vision that if providers could collaborate and share clinical information, mental health needs would resolve more quickly. How could we make this happen?
In 2019, we did the unthinkable: We partnered to establish a unique delivery system with a mission to disrupt the status quo and deliver a more progressive, data-driven model of mental health care, particularly for children and adolescents. We called it Aloft Integrated Wellness.
Case Study
“Brandon,” a 15-year-old white male patient, presents to the Aloft collaborative care model (CoCM) program with attention-deficit/hyperactivity disorder (ADHD) combined type, diagnosed at age 8; generalized anxiety disorder, diagnosed at age 10; and recurrent, moderate major depressive disorder, diagnosed at age 13. Brandon is taking oral methylphenidate extended release 72 mg every morning, oral fluoxetine 40 mg every day, and oral bupropion extended release 300 mg every day. He was hospitalized at the age of 10 years for homicidal ideation.
Brandon has a long history of behavioral issues both at school and home, including impulsive behavior, fixations on sexualized online content and video games, and emotional dysregulation. His school individualized education program includes a full-time one-on-one aide. Brandon has been treated by a therapist and psychiatrist, with little coordination between the providers, despite highly engaged parents. Neither of Brandon’s providers use measurement-based care or validated screening tools.
Brandon’s parents are frustrated by the lack of collaboration between medical professionals and spend much of their time acting as liaisons between providers. After learning about the CoCM program’s team-based approach, his parents seek access to the Aloft program.
At the time of enrollment into the CoCM, Brandon is missing school, isolating in his bedroom, and playing video games during the night. Conflicts at home are frequent and escalate quickly. In the past 6 months, the police have been called to his home 3 times to address physical aggression and verbal escalation. How do you proceed?
Our Story
In 2019, Aloft Integrated Wellness partnered with Core Physicians Pediatric and Adolescent Medicine to pilot a new model addressing mental health needs of younger patients, drawing from both integrated behavioral health and the CoCM. This model embodies the whole person approach, reducing the burden placed on the primary care team to assess, triage, and respond to mental health needs of patients. Through routine screening, the use of validated data, and provider collaboration, Aloft successfully prioritized early identification and responded to emerging behavioral health concerns. Outcome data demonstrated a significant reduction in ED use and a significant increase in access to care.
Aloft recognized that addressing the youth mental health crisis would require innovation and new models of care. The persistent shortage of child and adolescent psychiatrists places significant pressure on other health care providers to diagnose and manage psychiatric issues in children. Given that 75% of primary care visits include a behavioral health concern,1 Aloft began to explore integrated behavioral health care models as possible solutions. The CoCM brings behavioral health into primary care settings using a care manager (CM), a behavioral health clinician (BHC) with a master’s degree, and a consulting psychiatrist. This data-driven model requires regular use of validated screening instruments, such as the Pediatric Symptom Checklist 35-item, General Anxiety Disorder 7-item, or Patient Health Questionnaire 9-item, to identify clinical needs and track changes over time. Unlike other models of integrated care, the CoCM is financially sustainable using reimbursement codes published by the Centers for Medicare & Medicaid Services in 2015.
Figure. CoCM Fully Informed Care Plan
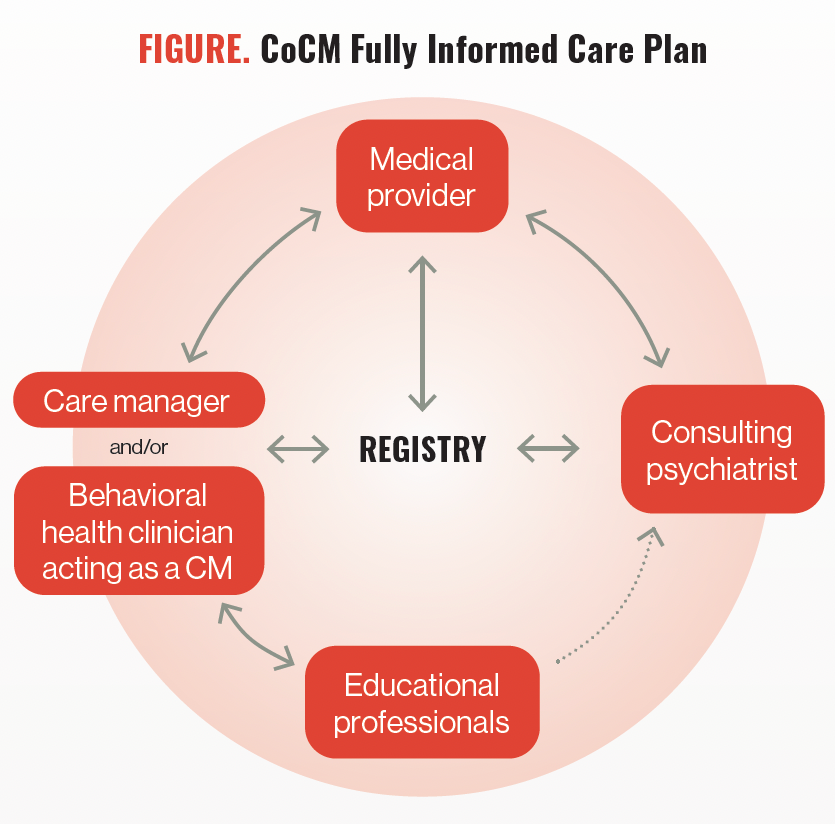
More good news came in 2020, when Aloft was awarded funding support through New Hampshire’s integrated delivery network to implement a pediatric integrated care pilot program. Aloft partnered with Core Physicians Pediatric and Adolescent Medicine to develop a collaborative care team, staffing their office with 2 BHCs and a CM. Charolette Lippolis Condon, DO, MPH, FAPA, joined the team as the child and adolescent consulting psychiatrist, bringing her years of experience in integrated care. Aloft innovated beyond the original CoCM by partnering with school personnel to build out a more complete picture of patients’ functioning in various domains. This adaptation led to a fully informed care plan, providing key information to the CoCM team (Figure).
Research on Collaborative Care
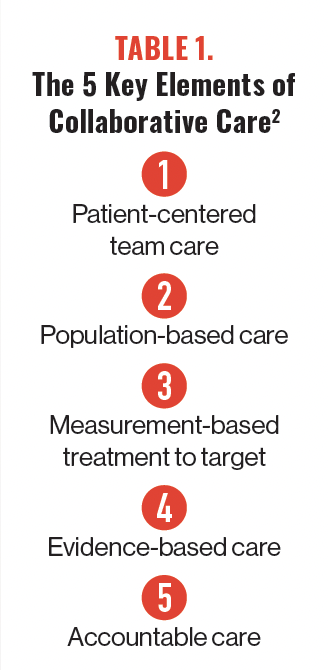
The American Psychiatric Association highlights 5 key elements of collaborative care (Table 1).2 The Advancing Integrated Mental Health Solutions (AIMS) Center IMPACT trial stated that “more than 90 randomized controlled trials and several meta-analyses have shown the CoCM to be more effective than usual care for patients with depression, anxiety, and other behavioral health conditions.” The CoCM also produces an estimated 6:1 long-term health care cost savings.3
CoCM Improves Mental Health Access
Barriers to accessing mental health care include social determinants of health, lack of insurance coverage, and the behavioral health workforce shortage. Patients are 5 times more likely to use out-of-network providers for mental health than for medical care, exacerbating access difficulties for resourced-limited and marginalized communities.4 More than half of all counties in the United States lack a single psychiatrist, and 158 million Americans live in a federally designated mental health shortage area.5
Table 1. The 5 Key Elements of Collaborative Care2
Collaborative care addresses the workforce shortage by streamlining access to care and using data to assess needs and outcomes. Psychiatrists are used in a consultative role, meeting weekly with the CM and primary care physician (PCP) to discuss 8 to 10 cases in an hour. The CM operates as the central hub of information, gathering input and data from the patient and, when appropriate, family members, school personnel, and outside providers. In most states, the CM is required to have “some behavioral health training.”6 This can occur on the job with trained staff with bachelor’s degrees, creating a new pipeline for workforce expansion.
CMs are directed by team members to provide psychoeducation and baseline interventions, such as reviewing sleep hygiene protocols and educating on lifestyle factors such as exercise and relaxation strategies. CMs also assist patients in addressing social determinant of health barriers such as food insecurity and transportation difficulties. Time spent is captured and billed using CoCM Current Procedural Terminology codes. In unintegrated, traditional settings, clinicians with master’s degrees often conduct these tasks as part of psychotherapy or between sessions in a nonreimbursable manner.
The BHC role is staffed by a licensed clinician with a master’s degree. Patients enrolled in the CoCM stay in the program for an average of 6 months and typically meet with the BHC for 5 to 8 sessions. Through emphasis on short-term, evidence-based models of care, such as cognitive behavioral therapy, motivational interviewing, and the Yale Supportive Parenting for Anxious Childhood Emotions model, patients engage in more targeted treatment. The use of measurement-based care and validated screening protocols supports the shorter-term duration of treatment under this model. Colocation is another consideration in CoCM implementation and maintenance. Although it is essential that the BHC is available for quick consultations with the team and warm handoffs during PCP visits, the consulting psychiatrist can be a remote participant and accessed using telemedicine.
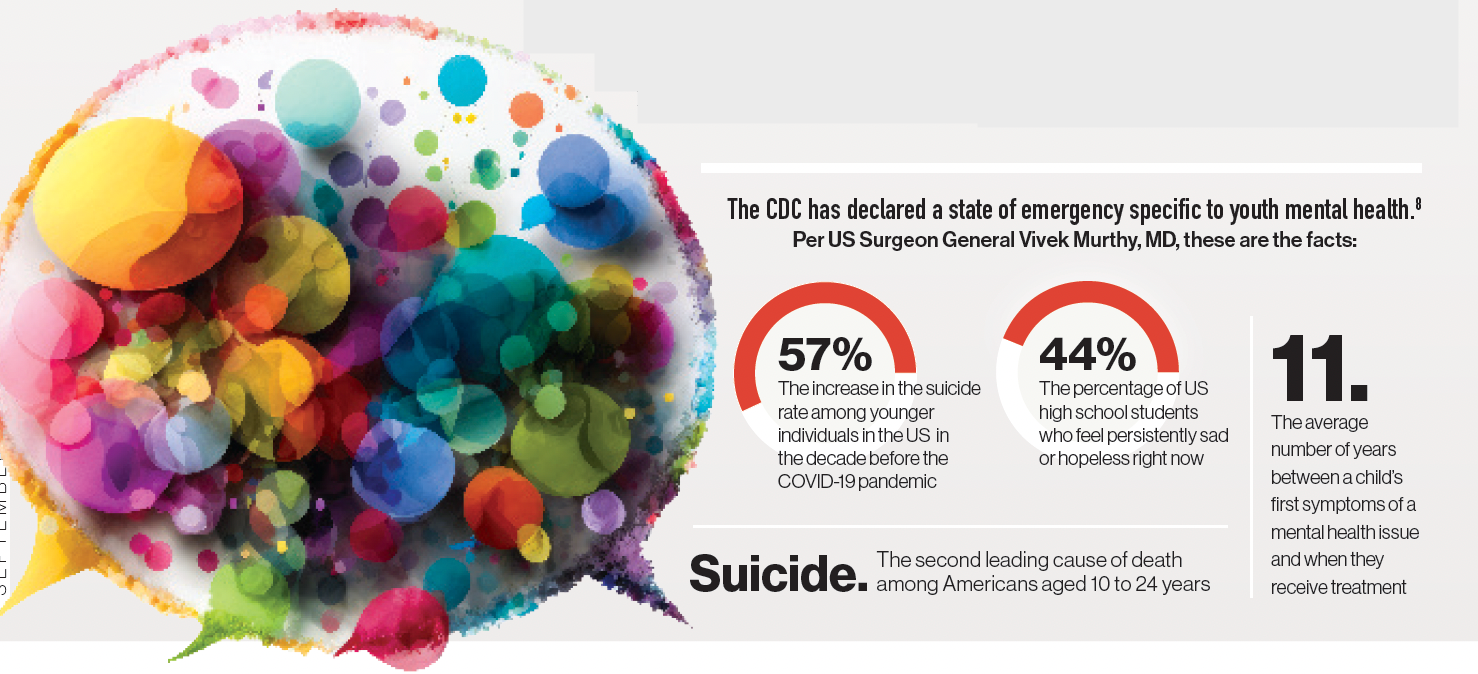
The CDC has declared a state of emergency specific to youth mental health.8
Per US Surgeon General Vivek Murthy, MD, these are the facts.
A Fully Integrated Measurement-Based Care Software
The CoCM harnesses the power of data to measure response to treatment and monitor change over time using validated screeners. Patients enrolled in the CoCM are screened at least once per month to monitor overall progress or flag regression. These data are accessed by the CoCM team in a product known as a registry.
In all areas of medicine, data-driven decision-making is the gold standard for best practices in patient care. Physical medicine utilizes laboratory values and imaging, along with clinical exam results, to inform providers about diagnoses and treatment plans; in mental health care, validated assessment tools provide the clinical data that, in addition to clinical interviews, allow for best practice decision-making and treatment planning. These validated assessments are not used as often as is recommended, in part because of the challenge of administering these tools to patients in an efficient and timely manner.
Aloft has partnered with Mirah, a behavioral health measurement-based care software solution. The Mirah platform streamlines measurement of patient assessment data and assists caseload management by acting as a patient population registry. Fully integrated into the practice’s electronic medical record, Mirah ensures seamless communication across the patient care team.
Case Study Conclusion During a handoff between the CM and pediatrician, a series of standardized questionnaires were selected and sent to the patient, parents, and school professionals through Mirah, an online HIPAA–compliant, measurement-based care platform (Table 2). The CM brought this information to the CoCM team for review. During the first CoCM team case review, the team evaluated Brandon’s presenting diagnoses of depression, ADHD, and anxiety. The team flagged the possibility of bipolar disorder. The CM sent additional validated assessments to gather additional information from the parents and patient, including the Mood Disorder Questionnaire for Parents of Adolescents and the Mood Disorder Questionnaire Adolescent Version.
Table 2. Examples of Standardized Questionnaires Sent Through Mirah

The team determined that Brandon met the criteria for bipolar disorder. Under the guidance of the consulting psychiatrist, the treating pediatrician prescribed new medication—quetiapine as his mood stabilizer—and discontinued the antidepressants and stimulant medications he had been taking, thereby appropriately managing his bipolar disorder. Metformin was later added after a 10-lb weight gain to manage antipsychotic-induced weight gain. Within weeks, Brandon’s mood stabilized. He began exercising regularly with his parents, conflict with his family reduced significantly, and he reported feeling much more in control of his emotions.
From initial referral to discharge, the CM coordinated with the school and parents, gathered vital diagnostic information, and tracked treatment response. With effective collaboration across providers, a shared care plan was developed and adjusted as needed. Brandon reengaged in school, family stress reduced significantly, and he began working a part-time job.
Concluding Thoughts
Aloft’s pilot program produced compelling results; on average, the CoCM team responded to referred patients within 2 days and conducted the first clinical visit within 2 weeks. Of the 550 referrals to the program, only 1 patient used the ED. In contrast, during the height of the COVID-19 pandemic, the CDC reported a 66% increase in youth mental health–related ED visits.7 The CoCM provides a team-based, multidisciplinary approach to assess and address mental health, bringing validated behavioral health resources to primary care and improving both access and outcomes for patients. Aloft now works with health care organizations around the country to implement CoCM and address the national mental health crisis.
Given the profound youth mental health crisis, integrated models of care such as CoCM offer real time solutions by enabling primary care to identify and address behavioral health concerns through routine screening and early intervention more efficiently. This model improves workforce efficiency by engaging psychiatrists in a consultative role and onboarding CMs to provide subclinical interventions and communicate across the provider team. Finally, the use of data through validated screening tools enables ongoing evaluation of treatment response and efficacy.
Ms Lyons is a licensed marriage and family therapist with 20 years of clinical practice experience. She is an adjunct professor in the Department of Human Development and Family Systems of the University of New Hampshire Graduate School in Durham. She is a cofounder of Aloft Integrated Wellness LLC. She also serves as a clinical advisor to Mirah. Mr Hillyard is a psychotherapist who has worked with children, adolescents, and families for 30 years. He is a cofounder of Aloft Integrated Wellness LLC. He also serves as a clinical advisor to Mirah and delivered a TEDx talk in 2019 called “Why Mental Health Check Ins Should Be a Part of a Child’s Wellness Visit.” Dr Lippolis Condon is a teleconsultant with Aloft Integrated Wellness and is board certified in both general and child and adolescent psychiatry. Throughout her medical career, she has worked at all levels of care in telehealth, consultation, and collaborative care programs as part of a larger mission to increase access to care and improve psychiatric treatment for children and their families on a larger scale.
References
1. Robinson PJ, Reiter JT. Behavioral Consultation and Primary Care: A Guide to Integrating Services. Springer International Publishing; 2006.
2. Learn about the collaborative care model. American Psychiatric Association. April 25, 2019. Accessed July 18, 2023. https://www.psychiatry.org/psychiatrists/practice/professional-interests/integrated-care/learn
3. Building the business case for team-based integrated care. University of Washington AIMS Center. Accessed June 6, 2023. https://aims.uw.edu/collaborative-care/building-business-case-cost-effectiveness-studies-collaborative-care
4. Melek S, Davenport S, Gray TJ. Addiction and mental health vs. physical health: widening disparities in network use and provider reimbursement. Milliman. November 19, 2019. Accessed May 30, 2023. https://www.milliman.com/-/media/milliman/importedfiles/ektron/addictionandmentalhealthvsphysicalhealthwideningdisparitiesinnetworkuseandproviderreimbursement.ashx
5. Mental health care health professional shortage areas (HPSAs). KFF. October 21, 2022. Accessed May 30, 2023. https://www.kff.org/other/state-indicator/mental-health-care-health-professional-shortage-areas-hpsas/
6. Behavioral health integration services. Centers for Medicare & Medicaid Services. March 2021. Accessed July 18, 2023. https://www.cms.gov/Outreach-and-Education/Medicare-Learning-Network-MLN/MLNProducts/Downloads/BehavioralHealthIntegrationPrint-Friendly.pdf
7. Leeb RT, Bitsko RH, Radhakrishnan L, et al. Mental health-related emergency department visits among children aged <18 years during the COVID-19 pandemic - United States, January 1-October 17, 2020. MMWR Morb Mortal Wkly Rep. 2020;69(45):1675-1680.
8. Protecting youth mental health: the U.S. surgeon general’s advisory. US Department of Health & Human Services. December 6, 2021. Accessed July 13, 2023. https://www.hhs.gov/sites/default/files/surgeon-general-youth-mental-health-advisory.pdf

Newsletter
Receive trusted psychiatric news, expert analysis, and clinical insights — subscribe today to support your practice and your patients.






