
Studies of mammalian species suggest that they possess awareness of self and even more subtle “human” qualities associated with empathy and social joy.

Studies of mammalian species suggest that they possess awareness of self and even more subtle “human” qualities associated with empathy and social joy.

Charles Dickens might well say of American psychiatry, “These are the best of times and the worst of times.”

Here's a sampling of Psychoeducational Resources with live links including those available from the NIMH (NIMH Schizophrenia_ and Learning About Healthy Living.

Schizophrenia is often characterized by lack of insight, treatment nonadherence, and poor prognosis. However, research suggests that patients with schizophrenia benefit immensely from learning about their illness.

Dr Angell and others may be right to claim that we should be concerned about the current practice of psychiatry. But the simple fact that mental illnesses seem to be common is not one of them.

Do you know someone that has fought the brave fight against serious mental illness? They deserve recognition and applause. Do nominate them or let them know of the Reintegration Awards.

While research suggests that cannabis use can induce an acute psychotic state, there is controversy about whether it may precipitate psychotic disorders, such as schizophrenia. These authors offer an update on this important issue and provide clinically useful recommendations.

Through patient self-management, mental health clinicians can transfer the focus from managing symptoms to allowing patients to live well in the context of their mental illness and medical comorbidities.

Critics of DSM-5 argue that the expansion of diagnostic criteria may increase the number of “mentally ill” individuals and/or pathologize “normal” behavior, and lead to the possibility that thousands-if not millions-of new patients will be exposed to medications which may cause more harm than good.

More and more research is being conducted in the US and abroad on the role of psychiatric pharmacogenomics in identifying new gene variants and in predicting treatment response to specific medications.

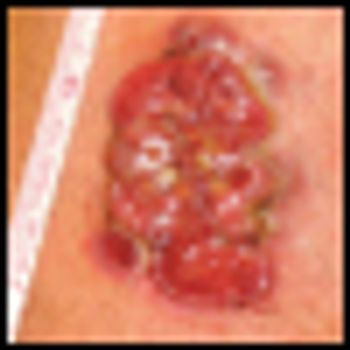
Skin diseases are not just a cosmetic issue; they are associated with a variety of psychological reactions that affect patients’ level of functioning and can produce agony for the family.

In psychiatry, it seems like our traditions are often ignored or discarded as being outdated. Do we not have some time-tested literature that is still relevant to our psychiatric times?

A study has reported a link between postpartum psychosis in women within 2 weeks after childbirth and a future risk of developing it.

The race to patent bio-tests for schizophrenia and depression: some say this initiative is destined to fail.

Some months ago, I received a stern admonition from my family doctor. My fasting blood sugar of 99 mg/dL was “right on the border”, he said, and I had better work on bringing it down. “But,” I protested, “when I was in medical school (in the 70s), the normal FBS range went up to 110 mg/dL!” "Well,” he replied a bit huffily, “they changed the criteria!”

The articles by Arline Kaplan and Hagop Akiskal, MD, in the November 2011 issue of Psychiatric Times highlight the race to patent bio-tests for schizophrenia and depression.
Biomarkers for mental disorders is a field whose time has come. Optimists will say within a few years, pessimists might say a decade or beyond.

Researchers have tried lots of different kinds of tests from EEGs to blood-based biomarkers. Now genetic tests are a very popular means of trying to understand different psychiatric disorders.

When I was a first-year resident, a revered supervisor of mine made the statement-half-facetiously-that, “In psychiatry, you can do biology in the morning and theology in the afternoon!”

Here, Dr Ira Steinman, discusses the concept behind "Beyond Pandora's Box: Exploring Integrative Approaches to Treating Psychosis."

A depot antipsychotic regimen is less likely to be discontinued than an oral dosage form . . .

Increased activity of the enzyme phospholipase A2 (PLA2) has been documented in schizophrenia and is now reported to occur in patients with temporal lobe epilepsy . . .

A bidirectional relationship between schizophrenia and epilepsy emerged from an analysis of a health insurance database . . .

This column has always been about the world of molecular mental health research. I revisit the technology in this column, now aimed at one of molecular neuropsychiatry’s most intractable, frustrating lines of research: the molecular/cellular basis of schizophrenia.

On the wide range of symptoms in schizophrenia, including alterations of the dopaminergic and/or glutamatergic systems, abnormal neurodevelopment, and the theory of immune system imbalance.